Wcauk.org
Achieving effective outcomes
in patients with overgranulation
Jackie Stephen-Haynes RGN DN DipH BSc (Hons) ANP. PG DipR PGDip Ed, Masters in Clinical Nursing
Consultant Nurse and Senior Lecturer in Tissue Viability for Worcestershire Primary Care Trusts and University of Worcester.
Stourport Health centre, Worcester St, Stouport on Severn, Worcestershire.DY13 8EH
Sylvie Hampton MA BSc (Hons) DpSN RGN,
Tissue Viability Consultant, Tissue Viability Consultancy Services. Eastbourne
WCA UK EDUCATION
Introduction
Many factors will delay wound healing (Hampton & Collins 2003), overgranulation is one of these factors that can delay
the wound healing process and can lead to a chronic wound.
Chronic wounds present tremendous challenges to the
The healing process associated with an acute wound is a dynamic
healthcare team. Unlike acute wounds that usually progress
one which can be divided into three phases (Dealey 2007):
neatly in a timely manner through the inflammation,
• Inflammation
proliferation and maturation phases of the healing process,
• Proliferation
chronic wounds deviate from this predictable sequence of
regeneration and repair (Krasner 1995) and more recently there has been increasing evidence for the effective treatment of over-granulation.
Stage of Inflammation
Overcoming the problem of overgranulation is difficult for health
Inflammation occurs immediately at the moment of tissue
care practitioners who need to assess the condition of the
damage, lasts a few days, five at most, and is the body's natural
granulation tissue to achieve good clinical outcomes for patients.
response to injury. As soon as the injury occurs the blood vessels in the wound bed constrict and a clot is formed.
In order to understand overgranulation, we must first
Once bleeding is halted, the blood vessels then dilate to allow
understand the wound healing process and therefore, the
essential cells; antibodies, white blood cells, growth factors,
aim of this booklet is to provide information on the healing
enzymes and nutrients to reach the wounded area. Because the
process and to describe how a wound becomes chronic and
vessels have dilated, fluid (exudates) can now easily leak out
colonised, providing a background to why a wound becomes
into the wound bed (Enoch & Price 2004; Enoch 2006). At this
over-granulated, how to avoid its occurrence and how to treat
stage neutrophils and macrophages commence their protective
it once it is established.
role and begin the orchestration of wound healing, moving
Achieving effective outcomes for patients with over-granulation
onto proliferation and it is this stage that chronicity can be
is possible and clinicians need the skills of assessment,
established, particularly if the wound becomes colonised or is
differential diagnosis, knowledge of the evidence to support
not treated appropriately. If chronic inflammation occurs, then
modern treatments and good communication skills to explain
there is a potential for future overgranulation. Certainly, chronic
this clearly to the patient.
inflammation will prevent the second stage (proliferation) from occurring (Moore 2004).
The wound healing process
Stage of proliferation
There is a great difference between chronic wound healing and acute wound healing and they are not interchangeable. An acute
The restoration of tissue and the redevelopment of tissue
wound will heal, without problems, in an orderly fashion unless
strength following wounding are initially achieved by the
the underlying pathology is not supportive of healing or the
formation of a myofibroblast-reticulin matrix which eventually
wound becomes clinically infected (Dealey 2007). The wound
disappears as the healing wound ages (Forrest 1982). At this
that does not heal in the normal way will become chronic and
point, the wound begins to fill and the new collagen fibrin
will then require art (knowledge and experience) and science
matrix is used by capillaries and cells as a ‘scaffolding' to build
(knowledge of research outcomes) in order to bring the wound
the new tissue. This building tissue contains macrophages,
back into the acute stage ready for healing.
fibroblast cells, and newly formed blood vessels, with a complex
WCA UK EDUCATION
collagen protein matrix. At this point, macrophages are probably the most important of the mediators of wound healing as they emit growth factors which attract fibroblasts and so initiates the next phase of wound healing.
The cells multiply within the matrix and fibroblasts in the granulation tissue "pull" on the matrix, causing the wound to contract, enabling the wound to move to the third stage - maturation. If clinical infection occurs at this point, the wound can develop a chronic inflammation and this inflammation can lead to tissue damage if it lasts too long (Midwood et al 2004) and it is this that will prevent the wound from continuing the healing process.
Although this has been simply explained here, chronicity is actually extremely complex and the subsequent chronic inflammation leads Matrix Metalloproteinases (MMPs) (which are so necessary to acute wound healing), to become a
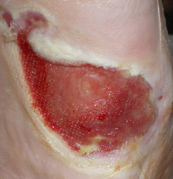
Figure 1. Granulation has smoothed out; the wound is just slightly moist and
damaging force in the chronic wound and therefore, will delay
is ready for the edges to contract. The stage of healing is maturation.
wound healing even further and prevent the wound from progressing to the stage of maturation.
These 3 stages should progress in an orderly (orchestrated) manner although the stages will overlap as can be seen in figure
Stage of maturation
2: This phase lasts 3 to 5 days
When granulation is achieved, the wound bed changes, becomes less ‘wet' and less ‘bumpy' with a smoother wound surface (figure 1). This is the final stage of wound healing and the epithelial cells can now grow into the centre of the wound and the wound fibres will contract the surface of the wound until it reaches closure. If this happens quickly there will be less scarring (Son et al 2005). The collagen that is laid down during the granulation period is now removed and replaced by a stronger collagen and the tissue beneath the scar and the scar itself, will go on remodelling for up to two years (Dealey 2007).
Figure 2 The 3 phases of wound healing. Each stage overlaps the previous stage and, if unable to pass from the acute phase will become chronic inflammation without healing.
WCA UK EDUCATION
If a problem, such as clinical infection occurs, then the wound
of required granulation tissue needed to replace the tissue
can ‘stick; in the 1st stage and this will then become chronic
deficit which often results in a peduncle (raised mass) above the
inflammation and the wound dynamics will change and the
wound (figure 4). It may be a difficult condition to manage and
wound will halt healing.
the presence of such tissue, as well as increasing the patient's risk of infection, will prevent or slow epithelial migration across
the wound and thus delay wound healing (Nelsen 1999).
Granulation tissue itself is composed largely of newly growing capillaries (angiogenesis) and is so called because the irregular surface is created by the capillaries looping together on the wound surface, giving the appearance of red lumps (or granules) throughout paler pink normal matrix. The appearance
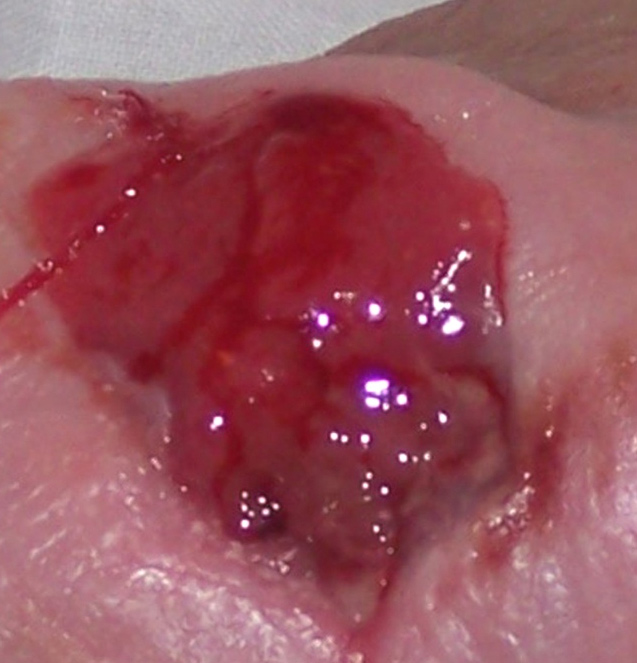
Figure 4. Overgranulation is a soft tissue that is ‘proud' of the wound (Peduncle) and minus the granules that represent granulation tissue. It will not progress toward healing.
Overgranulation is also known as hypergranulation, exuberant
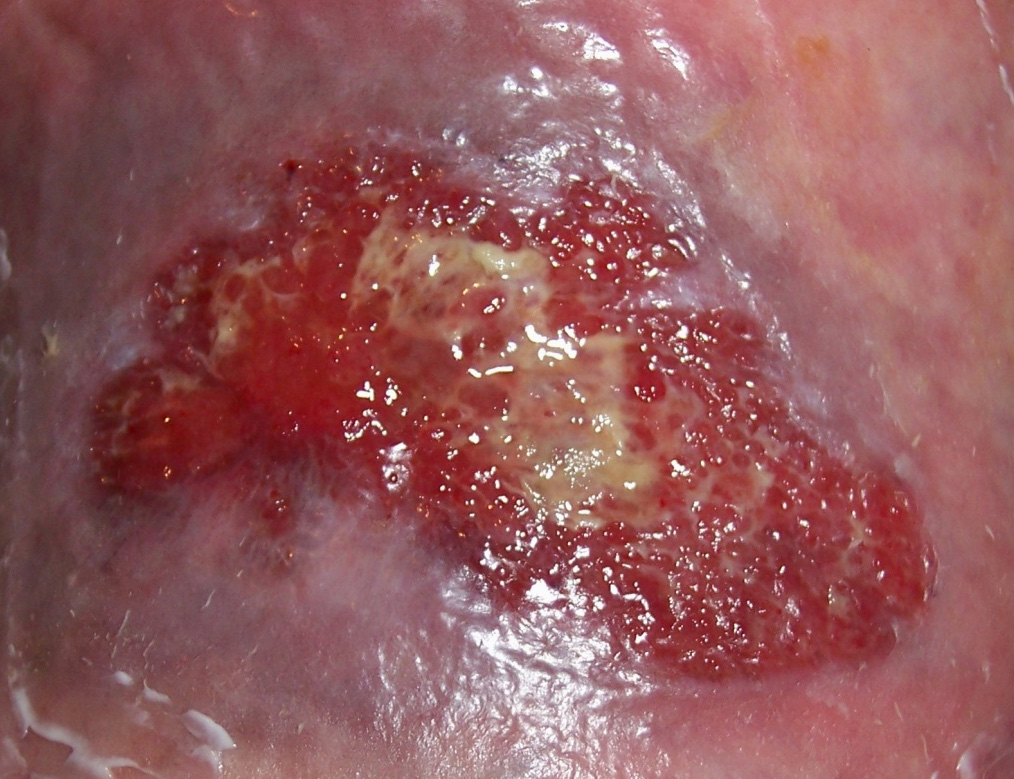
Figure 3. Granulation tissue consists of a pale base of matrix
granulation tissue, or proud flesh and usually presents in
and many capillaries looping together on the surface, forming
wounds healing by secondary intention. It is clinically recognised
‘lumps' that have the appearance of granules.
by its' friable red, often shiny and soft appearance that is above
is granular (figure 3), and naturally has the name granulation.
the level of the surrounding skin (Johnson & Lea 2007) and
If granulation is present in the wound it is an indication that
can be healthy (figure 5) or unhealthy (figure 6) tissue (Harris
healing is occurring and a dense network of capillaries, a high
& Rolstad 1994). There is some thought that this problem is
number of fibroblasts, macrophages and new formed collagen
associated with oedema of granulation tissue and this oedema
fibres will be present (Vuolo 2009).
may be associated with occlusive dressings that do not allow drainage of wound exudates (Vandeputte & Hoekstra 2006).
The oedema would be increased in the presence of bacterial
However, sometimes the granulation will ‘over grow' beyond
loading in the wound, whether that loading is associated with
the surface of the wound and this is called ‘Proud Flesh',
colonisation or with clinical infection. This oedema could
‘hypergranulation' or ‘overgranulation'. Overgranulation is
possibly be seen as a ‘healthy' overgranulation (figure 4) which is
defined as an excess of granulation tissue which is in excess
different to ‘unhealthy', infected and friable overgranulation.
WCA UK EDUCATION

However, whether healthy or unhealthy, the wound generally
Healthy overgranulation tissue presents as an overgrowth of
will not heal when the tissue is ‘proud' of the wound because
moist, pinky-red tissue (figure 5) that may bleed easily (Johnson
epithelial tissue will find it difficult to migrate across the surface
& Lea 2007) and unhealthy overgranulation tissue presents as
and contraction will be halted at the edge of the swelling.
either a dark red or a pale bluish purple uneven mass rising above the level of the surrounding skin which also bleeds very easily (figure 6). The healthy granulation tissue has the potential to reduce naturally and to eventually heal without intervention although this may take longer than if it is treated.
Particular care should be taken in differential diagnosis as an overgranulating wound can appear as similar to a malignancy wound, particularly a fungating wound (Harris & Rolstad 1994).
Overgranulation in diabetes
Soft tissue coverage of chronic diabetic ulcers can be particularly
troublesome because of the lack of adequate blood supply
available to the wound and this can form inadequate granulation
tissue (Younes et al 2006). Also, the person with diabetes is very
Figure 5. Healthy granulation tissue. Can be treated with pressure or topical
prone to clinical infection in wounds due to the inadequate
tape (Haelan tape) steroid cream or ointment.
delivery of oxygen and nutrients to the wound bed which increases the potential for abnormal tissue such as overgranulation.
Possible causes of overgranulation:
There is limited research relating to the cause of over-
granulation with several authors offer several suggestions. These
relate to 3 areas: inflammation, occlusion or cellular imbalance:
• Prolonged inflammation caused by infection or dressing
fibre irritant (Harris & Rolstad 1994; Nelsen 1999).Clinical
infection will halt the healing process and will increase
fluid loss and may contribute to overgranulation.
• Continued minor trauma or external friction. Reported
in Gastrostomy tubes and supra pubic catheter sites (Lyon
& Smith 2001; Hanlon & Heximer 1994).
• Over use of occlusive dressings is thought to have an
influence on overgranulation as it creates a hypoxic
environment that causes the body to produce more but
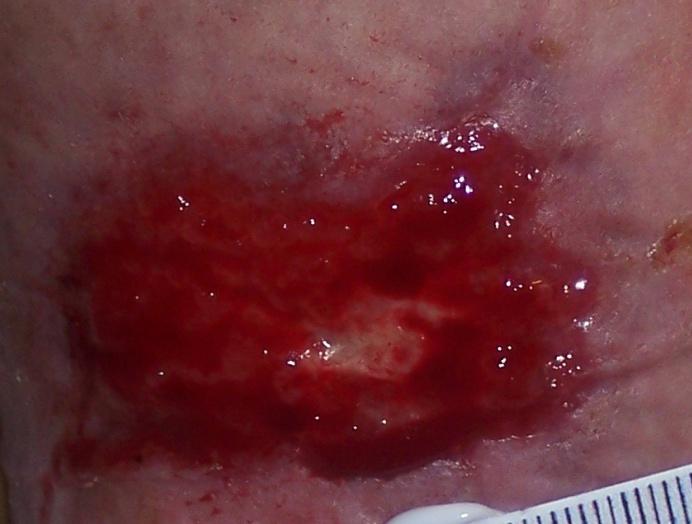
Figure 6. Unhealthy overgranulation. Extremely friable and obviously due to
immature blood vessels to compensate (Dealey 2007).
clinical infection, May require oral antibiotics and pressure or topical tape (Haelan tape) steroid cream or ointment.
WCA UK EDUCATION
• Occlusive dressings may keep the surface of the wound
extremely wet which could encourage oedema and swelling
in the wound bed (Vandeputte & Hoekstra 2006).
A malignancy may be mistaken for overgranulation and, if there is any suspicion that this is not normal tissue, the patient should
• Excessive exudates, possibly due to infection or chronic
be referred by the GP for a biopsy. There will be some clues:
colonisation, are also associated (Vandeputte & Hoekstra 2006).
• The overgranulation has been present for many months
• An imbalance between collagen synthesis and degradation
• It has a cauliflower appearance or is hard to touch
due to pathology within the patient (Sussman & Bates-
• It is growing outward beyond the wound margins
• It does not respond to any of the above treatments
Overgranulation is extremely common in horses, as their
Accurate assessment is important as the removal of malignant
leukocytes produce fewer mediators, initiating a weak
tissue could lead to significant blood loss and would have a negative
inflammatory response, which the causes the wound to become
rather than a positive impact on the wound and the patient.
chronic. This inhibits wound contraction and gives rise to the formation of exuberant granulation tissue (Wilmink & van
Treatment of overgranulation
Weeren 2005). A question could be asked - if low numbers or inactive leucocytes produce overgranulation in horses, could it
There are many treatment options for overgranulation with
also be a cause in humans and should we be testing for white
limited research to support their use or to clearly suggest
cell levels in humans with chronic wounds?
which is the most effective. This leads to a lack of overall consensus for treatment but broad principles for care should be
considered, see Fig 7.
Any wound assessment should include the following factors:
If the cause may be inflammation then consider securing any
(Stephen-Haynes 2010)
medical device such as gastrostomy, catheter tubing to minimise friction at the wound site.
• The environment
• A holistic assessment of the individual
A "wait and see" approach was suggested by Dunford (1999)
• Comprehensive assessment of the wound including history,
but the last 11 years has seen some significant developments
tissue, infection, peri wound area and edge of the wound
in this area of tissue viability and a more pro-active approach
• Consideration of the skin as a sensory organ
should be taken.
• Assessment of the patients knowledge and understanding of
Inflammatory response may be related to infection and the use
their wound and general condition
of an antibacterial dressing such as sliver, iodine cadexomer,
Particular assessment in relation to granulation should be to
honey, PHMB can assist with managing local colonization and
consider the most likely cause including inflammation, occlusion
reduce the potential and also reduce the overgranulated tissue
or cellular imbalance, as this may indicate an appropriate
(Leak 2002). It is important that infection is identified and
approach to treatment.
treated topically or systemically, depending on the spread of the infection, with care taken to avoid occlusion which will exacerbate the problem (EWMA 2006).
The earliest recommendation for treating overgranulation was foam, Harris and Rolstad (1994) reported the findings of a
WCA UK EDUCATION
prospective non-controlled correlation study with 10 patients
for the success of Tri-adcortyl in reducing overgranulation as
and 12 wounds using a polyurethane foam dressing to reduce
reducing the bacteria load would remove the infection that
overgranulation tissue. The results demonstrated a reduction in
stimulated the tissue to overgrow while the steroid reduces the
granulation tissue (p < 0.01). It was concluded that the pressure
inflammation that also stimulates overgrowth.
of the foam on the granulation tissue reduced the oedema
Lloyd-Jones (2006) reported resolution of overgranulation tissue
and flattened the overgranulation tissue. It is assumed that the
using a silver hydrofibre dressing, but this took some weeks
pressure of the foam on the granulation tissue reduces the
to resolve which is much longer than other treatments. The
oedema and flattens the overgranulation tissue and, when foam
author does, however, pose the question of whether the most
dressings were advocated, it was suggested that two pieces
appropriate silver dressing product was used in this study and if
of foam were applied to increase the pressure on the tissue
the use of silver products on overgranulation tissue is appropriate.
(Williams 1996; Rollins 2000; Carter 2003.)
With the length of time the overgranulation tissue took to resolve
Pressure from foam was then replaced by the suggestion of
it could be argued that the same result would have been achieved
double application of hydrocolloid. Controversially an occlusive
without any intervention or it may have been the pressure from
dressing is thought to be a possible cause of overgranulation
the outer dressing that resolved the overgranulation.
but potentially the pressure of the double application may reduce the excess tissue.
Haelan cream/Harlan tape
Morison et al (2007) notes that silver nitrate sticks are
Haelan tape is a transparent, plastic surgical tape (Blenderm;
traditional practice, reducing fibroblast production. This is
3M Healthcare, Loughborough), impregnated with 4 mg/
considered to be one of the most successful treatments
cm2 fludroxycortide (flurandrenolone), which al ows steady
for overgranulation and has produced good results in
distribution of the steroid to the af ected site. Fludroxycortide is
practice (Borkowski 2005). However, the use of silver nitrate
a fluorinated, synthetic, moderately potent corticosteroid. As with
directly reduces fibroblast proliferation and is therefore, not
other topical steroids, the therapeutic ef ect is primarily the result
recommended for prolonged or excessive use (Dealey 2007)
of its antiinflammatory, antimitotic and antisynthetic activities.
and should never be considered first-line therapy and should only ever be used with great care for the more stubborn area
An advantage of the steroid in a tape form is the capacity to
of granulation (Hampton 2007). This is particularly important
cut the tape to fit around tubes, e.g. percutaneous endoscopic
as chemical burns have been reported and more likely to
gastrostomy (PEG) tubes and supra-pubic catheters. Additionally,
occur with longer application times. When it is necessary, a
the pressure exerted by the tape while in situ may have a positive
topical barrier preparation such as petroleum jelly or white
ef ect on the reduction of overgranulation tissue. Importantly, the
soft paraffin should be applied to protect the normal skin
resolution was noted within 7 days or less by Johnson (2007) who
surrounding the area of overgranulation (Hampton 2007).
reported successful outcomes in 7 patients including post surgery, a lymphocele, dehisced abdominal wounds, venous leg ulceration,
Another highly successful method of treatment would be a
PEG and supra-pubic catheter sites. Similarly, Oldfield (2009)
short course of a topical steroid to suppress the inflammatory
reports successful treatment of an overgranulated surgical wound,
process (Carter 2003; Cooper 2007) and Tri-adcortyl was often
tracheostomy site, diabetic foot ulcer, peg insertion site and a stoma
the chosen steroid to be used in this case. However, it is no
site. Importantly, corticosteroids whilst fast acting is not licensed for
longer recommended for this purpose as it contains Auromycin,
use on open wounds. Haelen tape contains a low dose of steroid
an antibiotic, and it is indiscriminate use of such antibiotic
and is marketed specifically for the purpose of overgranulation.
therapy that may have initiated MRSA. Reducing the bacterial burden with Auromycin may be one of the possible reasons
WCA UK EDUCATION
Removal of overgranulation
Suggested treatment for overgranulation (Fig. 7)
Because granulation tissue is very delicate, it can sometimes be
Treatment
Treatment
removed by wiping with a cotton swab. However, this should only
be undertaken by a nurse experienced in wound care such as a
Over-granulation
Tissue Viability Nurse, as the wound could be traumatised and
healing could be further delayed. Surgical or conservative shape
Harris & Rolstad, (1994)
wound debridement is an option, however, this should only be
undertaken by a surgeon as it wil be cutting into live tissue with
Apply a foam dressing
a blood supply and could cause a clinical infection to occur.
To reduce moisture
non-occlusive dressing;
Extra pressure application using compression bandaging or firm fixation tape may help. However, this should be monitored
closely and if changes are not seen within a week, one of the
recommendation its
effect is debateable
above solutions should be considered. However, there is no literature to back up many of the above claims and the advice
is often based on anecdotal and expert opinion. Also, with time,
Topical corticosteroid
healthy overgranulation may resolve itself without intervention
granulation tissue
and the tissue only needs to be removed if epithelialisation is
Only if all else has
Morison et al (2007)
retarded and healing is impeded because the skin surface will
Silver nitrate pencil
restored during the remodelling or the maturation stage of healing (Moore 2004).
Antimicrobial and
Lloyd Jones (2006)
from the foamUndertaken in
Surgical excision
WCA UK EDUCATION
Prevention of overgranulation
Overgranulation is certainly recognised as a clinical problem
Overgranulation is a common problem encountered in wound
(Harris & Rolstad (1994), Williams (2006), Dealey (2007),
care. There are several potential options for treatment. Some
Vuolo (2009) and most clinicians feel the need to remove the
have an immediate short term effect but may have a longer
excess tissue. However, the limited evidence regarding the
term unfavourable effect e.g. silver nitrate application and
management of overgranulation tissue necessitate a level of
surgical excision, which may delay wound healing by reverting
clinical judgement for the management of each individual patient
the wound back to the inflammatory phase of healing.
to ensure that removal of the tissue is not actually harmful. If
Other products, such as foams and silver dressings may offer
the tissue is healthy or if it is malignant, removal of the tissue
some effect but have frequently been utilised as a long term
could cause harm and should be avoided. However, if the tissue
treatment, without clinical benefit. The more recent research
is unhealthy overgranulation, not removing it will place the
supporting Haelan cream and tape indicates is an efficacious
patient at increased risk of clinical infection. The simplest rule
and costeffective treatment for overgranulation in a variety of
would be to use occlusion (if it is a cause), short term only,
wound types. The future of treating overgranulation may lie with
providing protection, warmth and a hypoxic environment in the
surgical lasers since lasers can not only remove overgranulation
early stages at a time that is most required. Once granulation is
tissue but will also cauterize small blood vessels and are very
established, a less occlusive dressing could be selected.
selective, leaving healing cells alone while removing excess and
Another cause is thought to be infection (EWMA 2006), therefore
unhealthy tissue.
precautionary measures should be undertaken to ensure the
Notwithstanding, further research is required to establish
wound does not become chronically colonised or infected.
exactly why overgranulation occurs as the cause will indicate
The most successful method of prevention would be
the most appropriate prevention and treatment.
appropriate assessment and treatment of the wound, ensuring
The ability of the healthcare practitioners to assess and
that the chronic wound is taken back to an acute wound where
differentiate between healthy and unhealthy overgranulation
healing will occur and then clever selection of dressings that will
is essential in making informed clinical decisions on how to
prevent colonisation. Continued assessment will alert the nurse
achieve effective outcomes. In conclusion, the clinician should
to changes in the granulation status and immediate action will
not be concerned about overgranulation as it can be treated if
ensure that overgranulation does not become a problem.
it cannot be prevented.
WCA UK EDUCATION
References
Bates-Jenson, B (1997) Wound care products: A guide to choice. Nursing Homes (USA).November/December pp.47-54.
Borkowski, L (2005) G tube care: managing hypergranulation tissue. Nursing. Aug; 35(8):24
Carter, K (2003) Treating and managing pilonidal sinus disease Journal of Community Nursing July 17 (7) 28-33
Cooper, R (2007) Steroid therapy in wound healing. Free Paper. EWMA Conference. Glasgow.
Dealey, C (2007) The Care of Wounds: a guide for nurses 3rd edition. Wiley-Blackwell, Oxford. 1999
Enoch, S., Price, P (2004) Cellular, molecular and biochemical differences in the pathophysiology of healing between acute wounds, chronic wounds and woundsin the aged. www.worldwidewounds. Accessed 7.3.2010
Enoch, S (2006) ABC of wound healing: Wound assessment BMJ; 14(89) - 132 March ISSN 0966-6494
Dunford, C (1999) Overgranulation tissue. Journal of Woundcare. 8 (10) p506-7
EWMA (2006) Position document. Management of infection. London. MEP Ltd 2006. Topical management of infected grade 3 & 4 pressure ulcers. Moore, Z & Romanelli, M. p11-13
Forrest, L (1982) Current concepts in soft connective tissue wound healing. British Journal of Surgery 70(3) 133-140.
Hampton, S., Collins, F (2003) Tissue Viability a comprehensive guide. Whurr publications. London.
Hampton, S (2007) Understanding overgranulation in tissue viability practice. British Journal of Community Nursing, September 2007, vol./is. 12/9(S24-30), 1462-4753
Hanlon, M., Heximer, B (1994) Excess granulation tissue around a gastrostomy tube exit site with peritubular skin irritation. Journal Wound Ostomy Continence Nursing 21(2) p76-77
Harris, A., Rolstad, B. S (1994) Hypergranulation tissue: a non-traumatic method of management. Ostomy Wound Management 40 (5): 20-30
Johnson, S (2007) Haelan Tape for the treatment of overgranulation tissue. Wounds UK. Vol 3 Issue 3 http://www.wounds-uk.com/journal/0303_haelan_article.shtml. Accessed 7.3.2010
Johnson, S., Lea, K (2007) Overgranulation tissue, a new approach www.woundsuk.co.uk/downloads/./JohnsonSusanPosterfomatted.doc (accessed 12th January 2010.
Krasner, D (1995) Minimizing factors that impair wound healing: a nursing approach. Ostomy Wound Management. Jan-Feb; 41(1):22-6, 28, 30; quiz 31-2.
Leak, K (2002) PEG site infections: a novel use for Actisorb Silver 220 (562kb) British Journal of Community Nursing, 7(6), 14 Jun, pp 321 – 325
Lloyd-Jones, M (2006) Treating Overgranulation with a silver hydrofibre dressing. Wound Essentials 1: 116–8
Lyon, C., Smith, A.J (2001) Abdominal Stomas and Their Skin Disorders – An Atlas of Diagnosis and Management. Martin Dunitz Ltd, London
Midwood, K.S., Williams, L.V., Schwarzbauer, J.E (2004) Tissue repair and the dynamics of the extracellular matrix. The International Journal of Biochemistry & Cell Biology, 36(6): 1031-1037
Disclaimer: The viewes expressed in this document are those of the author(s) and not necessarily of the Wound Care Alliance UK.
WCA UK EDUCATION
Source: http://www.wcauk.org/downloads/booklet_overgranulation.pdf
London Knee Clinic Partial Knee Joint ReplacementPatient information brochure New mobility with a partial knee replacement This brochure has been written for patients, family mem-bers and all those who wish to know more about the partial replacement of a knee joint. It will answer basic questions, explain the principle of the implantation of a partial knee joint as well as the procedure, and relieve you of any misgiv-ings or fears you may have.
El boletín de los socios de la AATI Mayo 2016 En esta edición: EDITORIAL UNA VEZ MÁS, PROTAGONISTAS EN LA FERIA DEL LIBRO Y TAMBIÉN EN LA NOCHE DE BUENOS AIRES OTOÑO EN FRANCÉS AATI Y ABRATES: UN NUEVO PUENTE TENDIDO ENTRE CULTURAS TRADUCTORES E INTÉRPRETES EN LA CIDADE MARAVILHOSA CHRIS DURBAN Y SU GUÍA DE INTERPRETACIÓN LA AATI EN LA LINTERNA DEL TRADUCTOR VIDRIERA DE SOCIOS






