Carsten-tschoepe.de
European Heart Journal Advance Access published April 11, 2007
European Heart Journal
How to diagnose diastolic heart failure: a consensusstatement on the diagnosis of heart failure with normalleft ventricular ejection fraction by the Heart Failureand Echocardiography Associations of the EuropeanSociety of Cardiology
Walter J. Paulus1*, Carsten Tscho
¨pe2, John E. Sanderson3, Cesare Rusconi4, Frank A. Flachskampf5,
Frank E. Rademakers6, Paolo Marino7, Otto A. Smiseth8, Gilles De Keulenaer9, Adelino F.
Leite-Moreira10, Attila Borbe
´des11, Martin Louis Handoko1, Stephane Heymans12,
Natalia Pezzali4, Burkert Pieske13, Kenneth Dickstein14, Alan G. Fraser15, and Dirk L. Brutsaert9
1Laboratory of Physiology, VU University Medical Center, Van der Boechorststraat, 7, 1081 BT, Amsterdam, The Netherlands;2Charite´ Universita¨tskliniken, Campus Benjamin Franklin, Berlin, Germany; 3Keele University, Stoke-on-Trent, UK; 4S.OrsolaHospital, Brescia, Italy; 5University of Erlangen, Germany; 6University of Leuven, Belgium; 7Universita degli Studi delPiemonte Orientale, Novara, Italy; 8Rikshospitalet, Oslo, Norway; 9Middelheim Ziekenhuis, Antwerp, Belgium; 10Universityof Porto, Portugal; 11Institute of Cardiology UDMHSC, Debrecen, Hungary; 12University Hospital Maastricht, The Netherlands;13Georg-August-Universita¨t, Go¨ttingen, Germany; 14Stavanger University Hospital, Norway; and 15University of WalesCollege of Medicine, Cardiff, UK
Received 28 November 2006; accepted 23 February 2007
Diastolic heart failure (DHF) currently accounts for more than 50% of all heart failure patients. DHF is also
referred to as heart failure with normal left ventricular (LV) ejection fraction (HFNEF) to indicate that
HFNEF could be a precursor of heart failure with reduced LVEF. Because of improved cardiac imaging
and because of widespread clinical use of plasma levels of natriuretic peptides, diagnostic criteria for
Natriuretic peptides;
HFNEF needed to be updated. The diagnosis of HFNEF requires the following conditions to be satisfied:
Ejection fraction
(i) signs or symptoms of heart failure; (ii) normal or mildly abnormal systolic LV function; (iii) evidenceof diastolic LV dysfunction. Normal or mildly abnormal systolic LV function implies both an LVEF . 50%and an LV end-diastolic volume index (LVEDVI) ,97 mL/m2. Diagnostic evidence of diastolic LV dysfunctioncan be obtained invasively (LV end-diastolic pressure .16 mmHg or mean pulmonary capillary wedgepressure .12 mmHg) or non-invasively by tissue Doppler (TD) (E/E0 . 15). If TD yields an E/E0 ratio sug-gestive of diastolic LV dysfunction (15 . E/E0 . 8), additional non-invasive investigations are required fordiagnostic evidence of diastolic LV dysfunction. These can consist of blood flow Doppler of mitral valve orpulmonary veins, echo measures of LV mass index or left atrial volume index, electrocardiographic evi-dence of atrial fibrillation, or plasma levels of natriuretic peptides. If plasma levels of natriuretic peptidesare elevated, diagnostic evidence of diastolic LV dysfunction also requires additional non-invasive inves-tigations such as TD, blood flow Doppler of mitral valve or pulmonary veins, echo measures of LV massindex or left atrial volume index, or electrocardiographic evidence of atrial fibrillation. A similar strategywith focus on a high negative predictive value of successive investigations is proposed for the exclusion ofHFNEF in patients with breathlessness and no signs of congestion.
The updated strategies for the diagnosis and exclusion of HFNEF are useful not only for individual
patient management but also for patient recruitment in future clinical trials exploring therapies forHFNEF.
In 1998, the European Study Group on Diastolic Heart Failurepublished a set of criteria for the diagnosis of diastolic heartfailure (DHF).1 At that time, DHF was presumed to account
* Corresponding author. Tel: þ31 20 4448110; fax: þ31 20 4448255.
for approximately one-third of all patients with heart
E-mail address:
[email protected]
& The European Society of Cardiology 2007. All rights reserved. For Permissions, please e-mail:
[email protected]
W.J. Paulus et al.
failure and its natural history was considered to be more
remodelling are already occurring in HFNEF.38 Such an evol-
benign than systolic heart failure (SHF) with a lower mor-
ution has also been observed in hypertensive heart
tality and morbidity rate.2–7 Over the last two decades,
disease,39–42 especially in African43–45 and Asian46,47 popu-
these perspectives have changed substantially with an
lations. In many of these studies, interval clinical events,
increase in the prevalence of DHF from 38 to 54% of all
such as myocardial infarction, were, however, not reported
heart failure cases.8,9 Moreover, the prognosis of patients
or significantly higher39 in the patients, who subsequently
suffering from DHF is as ominous as the prognosis of patients
developed a depressed LVEF. An occasional (3.5%) evolution
suffering of SHF.10–15 Predisposing conditions for DHF are
to eccentric LV remodelling is also observed in patients
older age, female gender, diabetes and obesity, arterial
with hypertrophic cardiomyopathy,48 a disease characteri-
hypertension, and left ventricular (LV) hypertrophy.16,17
zed in its initial stages by concentric LV remodelling and
Even following a myocardial infarction, many elderly
prominent diastolic LV dysfunction. A small, serial echocar-
patients still present with DHF.18
diographic study of HFNEF patients observed in one-fifth of
Because of this epidemiological evolution towards a
the patients a decline in LVEF below 45% after a 3-month
predominance of DHF in western populations, a re-appraisal
follow-up period.49 Larger follow-up studies, preferably
of the original set of criteria for the diagnosis of DHF is
with sequential coronary angiograms, are required to inves-
required. This re-appraisal should address the critiques,
tigate whether HFNEF is indeed a precursor stage to HFREF
which have been phrased concerning the original set of
and to identify patient characteristics, such as female
criteria, and should accommodate new pathophysiological
gender,50 regular aerobic exercise,51 chronic alcohol inges-
insights, modern cardiac imaging technology, and the wide-
tion,52 genetic background,53 and comorbidities, such as
spread clinical use of heart failure biomarkers.
diabetes,54,55 that may prevent or retard the evolutionfrom HFNEF to HFREF.
Structural, functional, and molecular biological argu-
Heart failure with normal left ventricular
ments support the theory that clinical heart failure presents
ejection fraction or diastolic heart failure
and evolves not as a single syndrome but as two syndromes,one with depressed LVEF and other with normal LVEF and
Heart failure with normal LV ejection fraction (HFNEF) is
specific mechanisms responsible for diastolic LV dysfunction
frequently referred to as DHF because of the presence of
(Figure 1). Patients with SHF have eccentric LV hypertrophy
diastolic LV dysfunction evident from slow LV relaxation
in contrast to patients with DHF, who have concentric
and increased LV stiffness.19 Diastolic LV dysfunction,
LV hypertrophy56,57 as evident from the numerous studies,
however, is not unique to patients with DHF but also
which reported a high LV wall mass–volume ratio in DHF
occurs in heart failure patients with SHF, and in this last
and a low LV wall mass–volume ratio in SHF.58–61 Differences
group, it even correlates better with symptoms than
between DHF and SHF have also been reported at the
LVEF.20,21 Furthermore, although global LV systolic perform-
ultrastructural level:61 patients with DHF have a 50% larger
ance is preserved,22 HFNEF patients have reduced myo-
cardiomyocyte diameter than patients with SHF and myofila-
cardial tissue Doppler (TD) velocities23–28 and abnormal
mentary density is also higher in the myocardium of patients
ventriculo-arterial coupling.29,30 On the basis of these
with DHF. Cardiomyocytes isolated from biopsies of DHF and
observations, the distinction between DHF and SHF is chal-
SHF patients also differ functionally. In vitro cardiomyocyte
lenged,31,32 and heart failure is considered to be a single
resting tension is higher in DHF,62 and together with collagen
syndrome characterized by a progressive decline in systolic
volume fraction, this higher cardiomyocyte resting tension
performance appreciated better by TD velocities than by
significantly contributes to in vivo myocardial stiffness.
LVEF (Figure 1). The concept of a single syndrome is
The cytoskeletal protein titin63 likely accounts for this
reinforced by the unimodal distribution of LVEF in large
higher resting tension. Titin functions as a bidirectional
heart failure trials that recruited both patients with
spring responsible for early diastolic LV recoil64 and late
reduced and normal LVEF.33 According to the single syn-
diastolic resistance to stretch.65,66 Isoform expression of
drome hypothesis, diastolic LV dysfunction is of similar
titin differs in patients with SHF and DHF: in patients with
origin in all heart failure patients and consists primarily
SHF, titin isoform expression shifts towards the more compli-
of increased interstitial deposition of collagen and modified
ant isoform,67–69 whereas in patients with DHF the shift is
matricellular proteins.34,35 In the absence of a discrimina-
towards the less compliant isoform.61 Apart from distinct
tory role for diastolic LV dysfunction, patients presenting
isoforms of cytoskeletal proteins in the LV myocardium of
with heart failure without depressed LVEF are better
patients with SHF and DHF, expression patterns of matrix
characterized by the term ‘HFNEF'36 or the term ‘heart
metalloproteinases (MMPs) and tissue inhibitors of MMPs
failure with preserved left ventricular ejection fraction'37
(TIMPs) also differ. In the myocardium of hypertensive
than by the term ‘DHF'.
patients with DHF70 and in aortic stenosis,71 there is a
In the single syndrome hypothesis, the major difference
decreased matrix degradation because of downregulation
between the two ends of the spectrum [HFNEF and heart
of MMPs and upregulation of TIMPs, whereas in dilated car-
failure with reduced LVEF (HFREF)] is the degree of LV ven-
diomyopathy, there is an increased matrix degradation
tricular dilatation and shape change or LV remodelling.36
because of upregulation of MMPs.72 In patients with aortic
Thus, it is postulated that there is an evolution or pro-
stenosis, who develop a depressed LVEF, this balance
gression from HFNEF to HFREF with the onset of LV
between proteolysis and antiproteolysis shifts73 and impor-
remodelling. LV volumes measured by three-dimensional
tant cardiomyocyte degeneration occurs.74 Furthermore, in
echocardiography are indeed already increased in HFNEF
trabeculae of explanted human hearts, alterations of
patients compared with normal subjects after matching for
calcium handling have been observed which selectively
age, gender, and body size suggesting that early stages of
disturb relaxation and diastole.75–81 These alterations may
How to diagnose diastolic heart failure
Heart failure: a single or two syndromes? Listing of arguments favouring heart failure to be a single or two distinct syndromes.
also be more prominent in DHF. Finally, in clinical outcome
of pulmonary oedema. In the outpatient setting, however,
trials with pharmacological intervention, patients with DHF
complaints of breathlessness are frequently reported
have not responded as convincingly as patients with
without detectable signs of congestion. ‘Presence of signs
SHF,8,82 which suggests that different pathophysiological
or symptoms of congestive heart failure' as the first criter-
mechanisms may be operative.
ium for the diagnosis of HFNEF is therefore preferable to
For clarity, the terms HFNEF and HFREF will be used
‘presence of signs and symptoms of congestive heart
throughout the remaining part of this manuscript and,
failure'. The latter criterion is used by the National Heart,
respectively, replace the terms DHF and SHF. This use of
Lung, and Blood Institute's Framingham Heart Study.93
HFNEF and HFREF does not imply that the issue of heartfailure presenting as one or two syndromes is resolved.
Normal or mildly abnormal systolicleft ventricular function
Three obligatory conditions for heart failure
The presence of normal or mildly abnormal systolic LV func-
with normal left ventricular ejection fraction
tion constitutes the second criterion for the diagnosis of
Three obligatory conditions need to be satisfied for the diag-
HFNEF. Since LVEF of heart failure patients presents as a
nosis of HFNEF (Figure 2): (i) presence of signs or symptoms
unimodal distribution, the choice of a specific cut-off
of congestive heart failure; (ii) presence of normal or mildly
value remains arbitrary.33 The National Heart, Lung, and
abnormal LV systolic function, and (iii) evidence of diastolic
Blood Institute's Framingham Heart Study93 used an LVEF .
LV dysfunction.
50% as cut-off for normal or mildly abnormal systolic LVfunction and this cut-off value has meanwhile been usedor proposed by other investigators.60,94 In the present
Signs or symptoms of congestive heart failure
consensus document, an LVEF . 50% is also considered
Signs or symptoms of congestive heart failure include lung
consistent with the presence of normal or mildly abnormal
crepitations, pulmonary oedema, ankle swelling, hepatome-
systolic LV function. LVEF needs to be assessed in accordance
galy, dyspnoea on exertion, and fatigue. Different modes of
to the recent recommendations for cardiac chamber quanti-
presentation of dyspnea (i.e. effort related or nocturnal)
fication of the American Society of Echocardiography and
need to be distinguished.83 In HFNEF, breathlessness is
the European Association of Echocardiography.95 It is of
frequently the earliest symptom due to pulmonary conges-
importance to note that in HFNEF reduced long-axis shorten-
tion,84 whereas muscle fatigue is more prominent in HFREF
ing is frequently compensated for by increased short-axis
due to reduced cardiac output, impairment of vasodilator
capacity, and abnormalities of skeletal muscle metabolism.
As already demonstrated by Frank, Starling, and Wiggers
Breathlessness is especially difficult to interpret in elderly
and later re-appraised,96 LV relaxation depends on end-
and in obese, who represent a large proportion of the
systolic load and volume.97–101 The criterion of ‘presence
HFNEF population. Objective evidence of reduced exercise
of normal or mildly abnormal LV function' therefore needs
performance can be provided by metabolic exercise
to be implemented with measures of LV volumes. To
exclude significant LV enlargement,95 LVEDVI and LV
consumption (VO2max)85–89 (reduced VO2max , 25 mL/kg/
end-systolic volume index cannot exceed 97 mL/m2 and
min; low VO2max , 14 mL/kg/min) or by the 6 min walking
49 mL/m2, respectively.
test90–92 (marked limitation ,300 m). In the hospital
Another concern related to establishing normal or mildly
setting, signs and symptoms of congestive heart failure are
abnormal LV function deals with the time elapsed between
usually simultaneously present as many patients are
the clinical heart failure episode and the procurement of
hospitalized for decompensated heart failure or episodes
the LV systolic function data. According to the criteria of
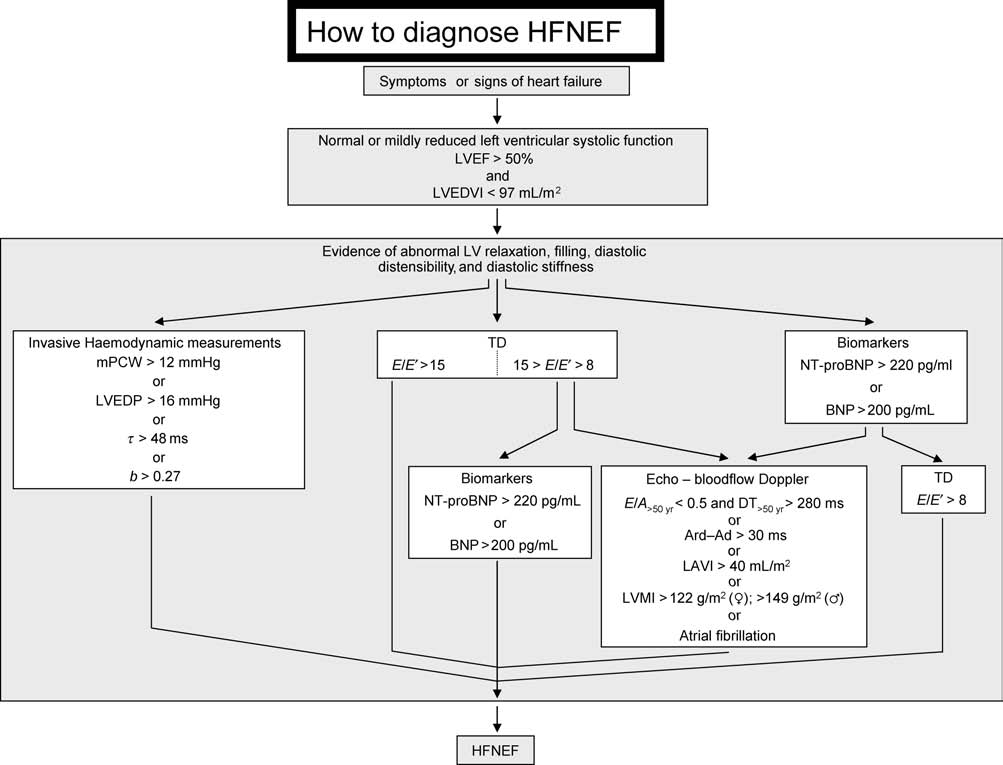
W.J. Paulus et al.
Diagnostic flowchart on ‘How to diagnose HFNEF' in a patient suspected of HFNEF. LVEDVI, left ventricular end-diastolic volume index; mPCW, mean
pulmonary capillary wedge pressure; LVEDP, left ventricular end-diastolic pressure; t, time constant of left ventricular relaxation; b, constant of left ventricularchamber stiffness; TD, tissue Doppler; E, early mitral valve flow velocity; E0, early TD lengthening velocity; NT-proBNP, N-terminal-pro brain natriuretic peptide;BNP, brain natriuretic peptide; E/A, ratio of early (E) to late (A) mitral valve flow velocity; DT, deceleration time; LVMI, left ventricular mass index; LAVI, leftatrial volume index; Ard, duration of reverse pulmonary vein atrial systole flow; Ad, duration of mitral valve atrial wave flow.
the National Heart, Lung, and Blood Institute's Framingham
hypothesis that measurement of diastolic LV dysfunction
Heart Study, a definite or probable diagnosis of HFNEF
was not required to make the diagnosis of HFNEF was
requires the information on LV systolic function to be
tested.60 Ninety-two per cent of patients with a history of
obtained within 72 h following the heart failure episode.93
heart failure, an LVEF . 50%, and evidence of LV concentric
This requirement may be obsolete because Doppler echocar-
remodelling had an elevated LV end-diastolic pressure and
diographic examinations of patients with hypertensive
all of them had at least one haemodynamic or Doppler echo-
pulmonary oedema performed sequentially at the time of
cardiographic index of abnormal LV relaxation, filling, or
hospital admission and following stabilization revealed iden-
diastolic stiffness. In this group of patients, acquisition of
tical LVEF and LV end-diastolic volume without evidence of
data on diastolic LV dysfunction therefore provided no
improvement of LV systolic function in the days following
additional diagnostic information and was therefore only
hospital admission.102
of confirmatory significance. As this study looked at patientswith a well-established history of heart failure, these resultscannot be extrapolated to patients presenting solely with
Evidence of abnormal left ventricular relaxation,
symptoms of breathlessness without a history or physical
filling, diastolic distensibility, and diastolic stiffness
signs suggestive of congestive heart failure. Nevertheless,
Do we need evidence of left ventricular dysfunction
this study among others,19,58–61 clearly demonstrates that
during relaxation or diastole?
evidence of concentric LV remodelling has important impli-
The need to obtain positive evidence of abnormal LV relax-
cations for the diagnosis of HFNEF and is a potential surro-
ation, filling, diastolic distensibility, and diastolic stiffness,
gate for direct evidence of diastolic LV dysfunction.94 The
as proposed in the original guidelines of the European
present consensus document (Figure 2) therefore considers
Study Group,1 has been challenged.60 Recognizing the diffi-
an LV wall mass index .122 g/m2 (C) or an LV wall mass
culties in the assessment of diastolic LV dysfunction, the
index .149 g/m2 (F) sufficient evidence95 for the diagnosis
How to diagnose diastolic heart failure
of HFNEF when TD yields non-conclusive results or when
by observations in hypertensives, in which the combined
plasma levels of natriuretic peptides are elevated.
use of these variables provided a semiquantitative estimateof LV end-diastolic pressure.120 Both studies measuredduration of reversed pulmonary vein atrial systole flow
Invasive assessment of left ventricular dysfunction
(Ard) and duration of mitral A wave flow (Ad) and used
during relaxation or diastole
their difference (Ard2Ad . 30 ms) to diagnose diastolic LV
Evidence of abnormal LV relaxation, filling, diastolic disten-
sibility, and diastolic stiffness can be acquired invasively
Because of the absence of pseudonormalization on TD
during cardiac catheterization. Invasively acquired evidence
lengthening velocity measurements, the use of blood flow
of diastolic LV dysfunction continues to be considered as pro-
Doppler measures of diastolic LV function is no longer rec-
viding definite evidence of HFNEF.1,19,93,94 Such evidence
ommended as a first-line diagnostic approach to diastolic
consists of a time constant of LV relaxation (t) .48 ms, an
LV dysfunction. Only when TD lengthening velocities are
LV end-diastolic pressure .16 mmHg or a mean pulmonary
suggestive but non-diagnostic or when plasma levels of
capillary wedge pressure .12 mmHg103–106 (Figure 2). The
natriuretic peptides are elevated does the simultaneous pre-
mathematics involved in deriving the time constant of LV
sence of a low E/A ratio and a prolonged DT or a prolonged
relaxation is explained in the appendix (Supplementary
Ard2Ad index provide diagnostic evidence of diastolic LV
material online). When LV end-diastolic pressure or pulmon-
dysfunction (Figure 2).
ary capillary wedge pressure is elevated in the presence of anormal LVEDVI, LV end-diastolic distensibility is considered
Tissue Doppler assessment of left ventricular dysfunction
to be reduced. LV diastolic distensibility refers to the posi-
during relaxation or diastole
tion on a pressure–volume plot of the LV diastolic
TD measures tissue velocity relative to the transducer with
pressure–volume relation107 in contrast to LV stiffness,
high spatial (mm) and temporal resolution (.100 s21).
which refers to a change in diastolic LV pressure relative
The most frequently used modality of TD is measurement
to diastolic LV volume (dP/dV ) and equals the slope of the
of LV basal (‘annular'), longitudinal myocardial shortening,
diastolic LV pressure–volume relation. A diastolic LV stiffness
or lengthening velocity. Measurements can be obtained
modulus .0.27 also provides diagnostic evidence of dias-
either at the septal or at the lateral side of the mitral
tolic LV dysfunction (see Supplementary material online,
annulus. As explained in the appendix (Supplementary
Appendix). The inverse of LV stiffness is LV compliance
material online), the peak systolic (S) shortening velocity
(dV/dP). Muscle stiffness (E) is the slope of the myocardial
and the early diastolic (E0) lengthening velocities are con-
stress–strain relation and represents the resistance to
sidered to be sensitive measures of LV systolic or diastolic
stretch when the myocardium is subjected to stress. Calcu-
lation of stress (s) requires a geometric model of the LV and
Especially, the ratio of early mitral valve flow velocity (E)
calculation of strain (e) an assumption of an unstressed LV
divided by E0 correlates closely with LV filling pressures.
dimension. Although muscle stiffness is generally considered
E depends on left atrial driving pressure, LV relaxation
to reflect the material properties of the myocardium and
kinetics, and age but E0 depends mostly on LV relaxation
therefore be insensitive to acute neurohumoral changes,
kinetics and age. Hence, in the ratio E/E0, effects of LV
recent clinical and experimental studies provided clear evi-
relaxation kinetics and age are eliminated and the ratio
dence for altered muscle stiffness following administration
becomes a measure of left atrial driving pressure or LV
of nitric oxide,108 endothelin-1,109 or angiotensin II.110 The
filling pressure. E0 can also be conceptualized as the
mathematics involved in deriving an LV or myocardial stiff-
amount of blood entering the LV during early filling,
ness modulus is outlined in the appendix (Supplementary
whereas E represents the gradient necessary to make this
material online).
blood enter the LV. A high E/E0 thus represents a highgradient for a low shift in volume. Information on LV filling
Blood flow Doppler assessment of left ventricular
pressures can also be derived from the time interval
dysfunction during relaxation or diastole
between the onset of E and the onset of E0 (TE2E0).133,134
Isovolumic LV relaxation time (IVRT), ratio of peak early (E)
When the ratio E/E0 exceeds 15, LV filling pressures are
to peak atrial (A) Doppler mitral valve flow velocity, decel-
elevated and when the ratio is lower than 8, LV filling press-
eration time (DT) of early Doppler mitral valve flow velocity,
ures are low.135 E/E0 is a powerful predictor of survival after
and ratio of pulmonary vein systolic (S) and diastolic (D) flow
myocardial infarction and E/E0 . 15 is superior as predictor
velocities were originally considered to be indicative of dias-
of prognosis than clinical or other echocardiographic vari-
tolic LV dysfunction if they exceeded specific cut-off values
ables.136 The close correlation between E/E0 and LV filling
indexed for age groups.1 These blood flow Doppler-derived
pressures has been confirmed in heart failure patients with
indices of diastolic LV dysfunction were subject of immedi-
depressed (,50%) or preserved LV ejection fraction137 and
ate critique111 and subsequently more carefully scrutinized
in patients with slow relaxation or pseudonormal early
in numerous studies.112–117 These studies are summarized
mitral valve flow velocity filling patterns.138 In the diagnos-
in the appendix (Supplementary material online) and
tic flow charts shown in Figures 2 and 3, the ratio E/E0 is
showed a variable outcome of blood flow Doppler-derived
therefore considered diagnostic evidence of presence of
indices in terms of their predictive value for HFNEF.
diastolic LV dysfunction if E/E0 . 15, and diagnostic
When combining mitral valve blood flow Doppler with
evidence of absence of HFNEF if E/E0 , 8. An E/E0 ratio
pulmonary vein blood flow Doppler,118 93% of patients
ranging from 8 to 15 is considered suggestive but non-
suspected of HFNEF showed evidence of diastolic LV dysfunc-
diagnostic evidence of diastolic LV dysfunction and needs
tion.119 The strength of a combined use of mitral flow
to be implemented with other non-invasive investigations
velocity and pulmonary vein flow velocity is also supported
to confirm the diagnosis of HFNEF (Figure 2). The proposed
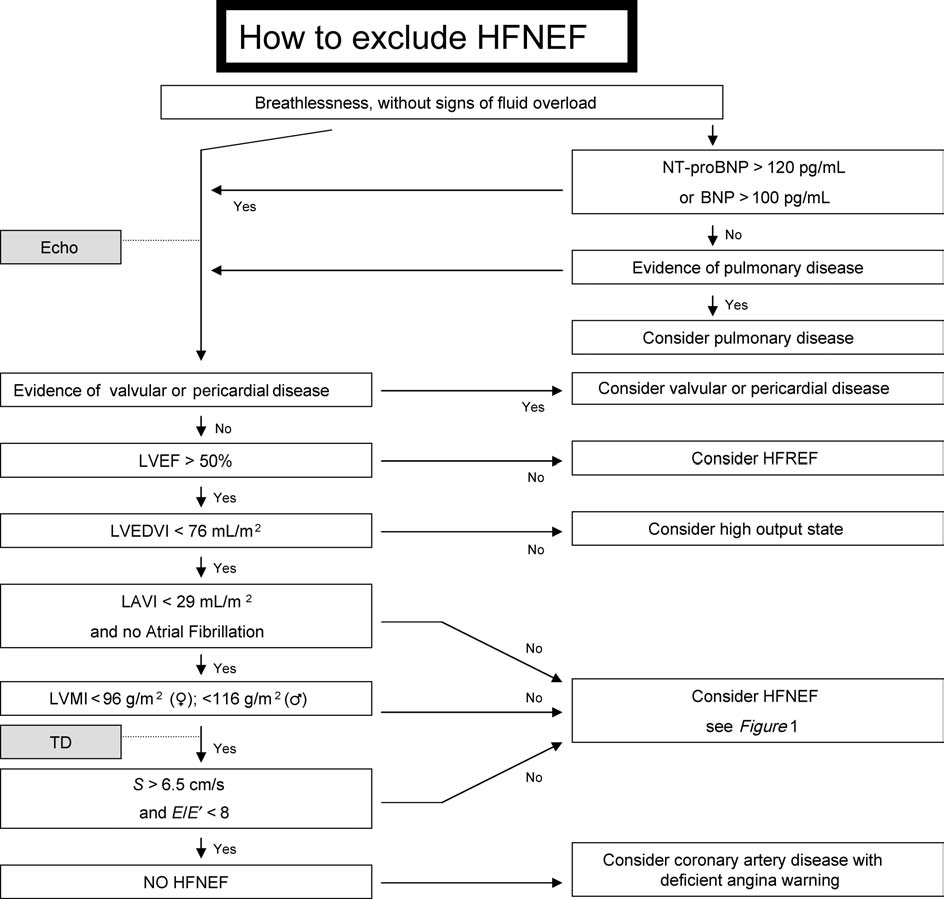
W.J. Paulus et al.
Diagnostic flow chart on ‘How to exclude HFNEF' in a patient presenting with breathlessness and no signs of fluid overload. S, TD shortening velocity.
E/E0 cut-off values are based on pulsed Doppler measure-
Left atrial volume measurements
ments and on averaged velocities of lateral and septal
A left atrial volume indexed to body surface area (¼ left atrial
mitral annulus.
volume index) .32 mL/m2 was first recognized in the elderlyas a strong predictor (P ¼ 0.003) of a cardiovascular eventwith a higher predictive value than other echocardiographi-
Strain and strain rate imaging
cally derived indices such as LV mass index (P ¼ 0.014) or LV
TD-derived strain rate and strain measurements are new
diastolic dysfunction (P ¼ 0.029).140 In a population-based
quantitative indices of regional intrinsic cardiac defor-
study, left atrial volume index was also strongly associated
mation139 and are presumed to be independent of transla-
with the severity and duration of diastolic LV dysfunction:
the left atrial volume index progressively increased from a
Assessment of regional deformation obviously implies that
value of 23 + 6 mL/m2 in normals to 25 + 8 mL/m2 in mild
all myocardial segments are to be investigated to rule out
diastolic LV dysfunction, to 31 + 8 mL/m2 in moderate dias-
diastolic LV dysfunction. In contrast, TD E/E0 interrogates
tolic LV dysfunction, and finally to 48 + 12 mL/m2 in severe
global LV performance and is therefore preferred over
diastolic LV dysfunction.141 Left atrial volume index was
strain and strain rate measurements in the diagnostic flow-
therefore proposed as a biomarker of both diastolic LV dys-
charts of HFNEF (Figures 2 and 3). Potential future use of
function and cardiovascular risk.142,143 A raised left atrial
strain and strain rate imaging for the assessment of diastolic
volume index (.26 mL/m2) has recently been recognized as
LV dysfunction is further highlighted in the appendix
a relatively load-independent marker of LV filling pressures
(Supplementary material online).
and of LV diastolic dysfunction in patients with suspectedheart failure and normal LVEF.116 In these patients, left
How to diagnose diastolic heart failure
atrial volume index is a more robust marker than left atrial
predictive value was aimed for when choosing the cut-off
area or left atrial diameter.144,145 For these reasons, the
values of NT-proBNP (220 pg/mL; Roche Diagnostics) and of
present consensus document considers a left atrial volume
BNP (200 pg/mL; Triage Biosite). For the exclusion of
index .40 mL/m2 to provide sufficient evidence of diastolic
HFNEF (Figure 3), a high negative predictive value was
LV dysfunction when the E/E0 ratio is non-conclusive (i.e.
aimed for and the respective cut-off values of NT-proBNP
15 . E/E0 . 8) or when plasma levels of natriuretic peptides
(120 pg/mL) and of BNP (100 pg/mL) were adjusted accord-
are elevated (Figure 2). Similarly, a left atrial volume index
ingly. NT-proBNP values of 120 and 220 pg/mL yielded,
,29 mL/m2 is proposed as a prerequisite to exclude
respectively, a negative predictive value of 93% and a
HFNEF (Figure 3). Left atrial volume index values of 29 and
positive predictive value of 80%.146 BNP values of 100
40 mL/m2 correspond, respectively, to the lower cut-off
and 200 pg/mL yielded, respectively, a negative predictive
values of mildly abnormal and severely abnormal LA size in
value of 96% and a positive predictive value of 83%.160
the recent recommendations for cardiac chamber quantifi-
Cut-off values of NT-proBNP were derived from ROC analysis
cation of the American Society of Echocardiography and the
performed in HFNEF patients presenting with exertional dys-
European Association of Echocardiography.95 The conduit,
pnoea.146 An ROC analysis for BNP in HFNEF patients pre-
reservoir, and pump functions of the left atrium in normal
senting with exertional dyspnoea has not been reported.
and pathophysiological conditions are further explained in
Cut-off values of BNP were therefore derived from ROC
the appendix (Supplementary material online).
analysis performed in HFNEF patients presenting in theemergency room with acute heart failure.160 As cut-off
Heart failure biomarkers: the natriuretic peptides
values of NT-proBNP and BNP were derived from different
Atrial natriuretic peptide (ANP) and brain natriuretic
HFNEF subgroups, their respective magnitudes and ranges
peptide (BNP) are produced by atrial and ventricular myo-
cannot be compared. To achieve satisfactory positive pre-
cardium in response to an increase of atrial or ventricular
dictive values, the diagnostic cut-offs of NT-proBNP and
diastolic stretch and their secretion results in natriuresis,
BNP had to be raised to a level, at which sensitivity drops
vasodilation, and improved LV relaxation. Cardiac myocytes
below 80%. This results from the overlap of NT-proBNP and
produce pro-BNP, which is subsequently cleaved in the blood
BNP values between controls and HFNEF patients, especially
into NT-proBNP and BNP.
when the HFNEF patients present with exertional dys-
In patients with HFNEF,146,147 NT-proBNP values correlate
pnoea.117 Natriuretic peptides are therefore recommended
with early diastolic LV relaxation indices, such as the time
mainly for exclusion of HFNEF and not for diagnosis of
constant of LV relaxation (t), late diastolic LV relaxation
HFNEF. Furthermore, when used for diagnostic purposes,
indices, such as LV end-diastolic pressure, and the LV stiff-
natriuretic peptides do not provide diagnostic stand-alone
ness modulus. BNP and NT-proBNP values also vary with
evidence of HFNEF and always need to be implemented
the degree of LV diastolic dysfunction: progressively higher
with other non-invasive investigations.
values were observed in patients with a mitral valve flowvelocity pattern of impaired LV relaxation, pseudonormali-
Cardiac magnetic resonance
zation, or restriction.117,148 The area under the receiver
The specific advantage of cardiac magnetic resonance (CMR)
operating characteristics (ROC) curve of NT-proBNP (0.83)
over echocardiography is the possibility to acquire images in
equalled the area observed for LV end-diastolic pressure
any selected plane or along any selected axis. This makes
(0.84) and exceeded the area observed for an abnormal TD
CMR the gold standard for LV volume, LA volume, and LV
E0/A0 ratio (0.81).146 Combining NT-proBNP with the E/E0
mass measurements.161,162 A routine CMR exam in the
ratio increased the area under the ROC curve from 83
setting of heart failure will acquire the following images:
to 95%.146 In contrast to its usefulness in symptomatic iso-
cine images (same slice over the cardiac cycle) with a set
lated diastolic LV dysfunction, natriuretic peptides were a
of contiguous short-axis slices, covering the entire heart
suboptimal screening test for preclinical diastolic LV
from base to apex and a set of long-axis slices (two, three,
and four chamber). CMR can provide a whole range of LV
In normal individuals, the concentration of NT-proBNP
filling parameters which are identical or nearly identical to
rises with age and is higher in women than in men.150 BNP
those obtained with echocardiography. As such, CMR is a
and NT-proBNP levels can be influenced by comorbidities
valid alternative for those patients who do not have an ade-
such as sepsis,151 liver failure,152 or kidney failure.153,154
quate echocardiographic image quality to reliably obtain
Plasma levels of BNP rise independently of LV filling press-
these parameters. Moreover, CMR constitutes not only a
ures once glomerular filtration rate falls below 60 mL/min.
valid alternative to echocardiography but could also be
Furthermore, BNP and NT-proBNP plasma levels do not
the first-choice technique if small changes in LA or LV
exclusively reflect left atrial distension but can also rise as
volumes and in LV mass are expected (e.g. when evaluating
a result of right atrial distension. The latter is especially
progression of disease or reaction to therapy). Finally,
important when pulmonary hypertension occurs as a result
several morphological and functional parameters such as
of chronic obstructive pulmonary disease,155 pulmonary
tissue characterization or LV diastolic untwisting can only
embolism,156 or mechanical ventilation.157 Finally, obesity
be assessed by CMR. These parameters contain important
lowers BNP levels158,159 and lower cut-off values have to
novel information for the identification of ischaemic, inflam-
be used once body mass index exceeds 35 kg/m2.
matory, or infiltrative myocardial disease and for the evalu-
The flowcharts for the diagnosis or exclusion of HFNEF
ation of diastolic LV dysfunction. Further details on the use
(Figures 2 and 3) do not consider an elevated BNP or
of CMR are available in the appendix (Supplementary
NT-proBNP to provide sufficient evidence for diastolic LV
material online).
dysfunction and require additional non-invasive examina-
Because of limited availability of CMR facilities, CMR is
tions. For the diagnosis of HFNEF (Figure 2), a high positive
currently considered to be a research tool and therefore
W.J. Paulus et al.
not included in the diagnostic flowcharts of HFNEF. As the
becomes the most likely cause of breathlessness. If an echo-
clinical use of CMR is expanding and starting to address dias-
cardiogram confirms the absence of valvular or pericardial
tolic LV dysfunction,163 indices of diastolic LV dysfunction
disease, LV volumes and LVEF should be measured in accord-
derived from CMR will probably have to be included in
ance to the recent recommendations of the American
future diagnostic strategies of HFNEF.
Society of Echocardiography and the European Associationof Echocardiography.95 If LVEF exceeds 50%, if LVEDVI is,76 mL/m2, and if the patient has no atrial fibrillation,
How to diagnose heart failure with normal
atrial dilatation, LV hypertrophy, low TD S or high TD E/E0,
left ventricular ejection fraction
the diagnosis of HFNEF is ruled out.
This consensus statement on ‘How to diagnose DHF?' retainsa diagnostic strategy of three requirements that need to be
satisfied to diagnose HFNEF (Figure 2). These requirementsare: (i) signs or symptoms of congestive heart failure;
As HFNEF currently accounts for more than 50% of all heart
(ii) normal or mildly abnormal systolic LV function, and (iii)
failure patients and as the prevalence of HFNEF in the heart
evidence of diastolic LV dysfunction. Since many patients
failure population rises by �1% a year,8 an updated set of
with HFNEF present with breathlessness and no signs of
diagnostic criteria for HFNEF is required. The diagnostic
fluid overload, symptoms are considered sufficient clinical
flowcharts on HFNEF proposed in this consensus statement
evidence to suggest the presence of congestive heart
provide a strategy on ‘How to diagnose HFNEF' (Figure 2)
failure. A LVEF of 50% is proposed as cut-off value of
and on ‘How to exclude HFNEF' (Figure 3). The diagnostic
mildly abnormal LV systolic function and an LVEDVI of
strategy on ‘How to diagnose HFNEF' is specifically intended
97 mL/m2 as cut-off value of the absence of significant LV
for patients suspected of having HFNEF and is primarily
enlargement. Invasive diagnostic evidence of diastolic LV
based on the positive predictive value of successive
dysfunction can be obtained by measuring the time constant
examinations. The diagnostic strategy on ‘How to exclude
of LV relaxation, LV end-diastolic pressure, pulmonary
HFNEF' is proposed for patients presenting with breathless-
capillary wedge pressure, or the LV stiffness modulus. Non-
ness and no physical signs of fluid overload and is mainly
invasive diagnostic evidence of diastolic LV dysfunction
based on the negative predictive value of successive
is preferably derived from myocardial TD (E/E0 . 15). If
examinations. These updated strategies for the diagnosis
myocardial TD yields values suggestive but non-diagnostic
of HFNEF should be helpful not only for individual patient
for diastolic LV dysfunction (15 . E/E0 . 8), TD needs to be
management but also for patient selection of future clinical
implemented with other non-invasive investigations to
trials looking at treatments for HFNEF.
provide diagnostic evidence of diastolic LV dysfunction.
These non-invasive investigations can consist of: (i) a
Supplementary material
blood flow Doppler of mitral valve flow velocity (E/A ratioand DT combined), or of pulmonary vein flow velocity
Supplementary material is available at European Heart
(Ard2Ad index); (ii) an echocardiographic measure of LV
Journal online.
mass index or of left atrial volume index; (iii) an electrocar-diogram with evidence of atrial fibrillation; and (iv) a
determination of plasma BNP or NT-proBNP. If plasmaNT-proBNP . 220 pg/mL or BNP . 200 pg/mL, diagnostic
The authors gratefully acknowledge the thoughtful comments of the
evidence of diastolic LV dysfunction also requires additional
members of the board of the Heart Failure and Echocardiography
non-invasive investigations, which can consist of: (i) TD (E/E0
Associations of the European Society of Cardiology.
ratio); (ii) a blood flow Doppler (E/A ratio and DT combined;Ard2Ad index); (iii) echo measures of LV mass index or left
Conflict of interest: none declared.
atrial volume index; and (iv) electrocardiographic evidenceof atrial fibrillation. The proposed use of different echocar-
diographic techniques, which includes measures derivedfrom mitral valve flow velocity (E/A, DT), pulmonary vein
1. European Study Group on Diastolic Heart Failure. How to diagnose dias-
flow velocity (Ard2Ad), and TD (E0), allows for a com-
tolic heart failure. Eur Heart J 1998;19:990–1003.
prehensive non-invasive assessment of LV relaxation, LV
2. Echeverria HH, Bilsker MS, Myerburg RJ, Kessler KM. Congestive heart
failure: echocardiographic insights. Am J Med 1983;75:750–755.
diastolic stiffness, and LV filling pressures.164
3. Dougherty AH, Naccarelli GV, Gray EL, Hicks C, Goldstein RA. Congestive
heart failure with normal systolic function. Am J Cardiol 1984;54:778–782.
How to exclude heart failure with normal
4. Soufer R, Wohlgelernter D, Vita NA, Amuchestegui M, Sostman HD,
left ventricular ejection fraction
Berger HJ, Zaret BL. Intact systolic left ventricular function in clinicalcongestive heart failure. Am J Cardiol 1985;55:1032–1036.
HFNEF is frequently a difficult differential diagnosis in a
5. Cohn JN, Johnson G. Heart failure with normal ejection fraction.
The V-HeFT Study. Circulation 1990;81:III-48–53.
work-up for breathlessness in the absence of signs of fluid
6. Wheeldon NM, Clarkson P, MacDonald TM. Diastolic heart failure.
overload. A strategy is therefore proposed to exclude
Eur Heart J 1994;15:1689–1697.
HFNEF (Figure 3). If a patient with breathlessness and no
7. Vasan RS, Benjamin EJ, Levy D. Prevalence, clinical features and
signs of fluid overload has a NT-proBNP , 120 pg/mL or a
prognosis of diastolic heart failure: an epidemiologic perspective.
J Am Coll Cardiol 1995;26:1565–1574.
BNP , 100 pg/mL, any form of heart failure is virtually
8. Owan TE, Hodge DO, Herges RM, Jacobsen SJ, Roger VL, Redfield MM.
ruled out because of the high negative predictive value of
Trends in prevalance and outcome of heart failure with preserved
the natriuretic peptides,146,160 and pulmonary disease
ejection fraction. N Engl J Med 2006;355:251–259.
How to diagnose diastolic heart failure
9. Abhayaratna WP, Marwick TH, Smith WT, Becker NG. Characteristics of
for the diagnosis and classification of heart failure. Eur J Heart Fail
left ventricular diastolic dysfunction in the community: an echocardio-
graphic survey. Heart 2006;92:1259–1264.
29. Kawaguchi M, Hay I, Fetics B, Kass DA. Combined ventricular systolic and
10. Cleland JG, Swedberg K, Follath F, Komajda M, Cohen-Solal A,
arterial stiffening in patients with heart failure and preserved ejection
Aguilar JC, Dietz R, Gavazzi A, Hobbs R, Korewicki J, Madeira HC,
fraction. Implications for systolic and diastolic reserve limitations.
Moiseyev vs, Preda I, van Gilst WH, Widimsky J, Freemantle N,
Eastaugh J, Mason J; Study Group on Diagnosis of the Working Group
30. Vinereanu D, Nicolaides E, Boden L, Payne N, Jones CJ, Fraser AG.
on Heart Failure of the European Society of Cardiology. The EuroHeart
Conduit arterial stiffness is associated with impaired left ventricular
Failure survey programme—a survey on the quality of care among
subendocardial function. Heart 2003;89:449–450.
patients with heart failure in Europe Part 1: patient characteristics
31. Sanderson JE. Diastolic heart failure: fact or fiction? Heart 2003;89:
and diagnosis. Eur Heart J 2003;24:442–463.
11. Owan TE, Redfield MM. Epidemiology of diastolic heart failure. Prog
32. Burkhoff D, Maurer SM, Packer M. Heart failure with a normal ejection
Cardiovasc Dis 2005;47:320–332.
fraction, is it really a disorder of diastolic function? Circulation 2003;
12. Yancy CW, Lopatin M, Stevenson LW, De Marco T, Fonarow GC, for the
Adhere Scientific Advisory Committee Investigators. Clinical presen-
33. Solomon SD, Anavekar N, Skali H, McMurray JJ, Swedberg K, Yusuf S,
tation, management, and in-hospital outcomes of patients admitted
Granger CB, Michelson EL, Wang D, Pocock S, Pfeffer MA, for the Cande-
with acute decompensated heart failure with preserved systolic func-
sartan in Heart Failure Reduction in Mortality (CHARM) Investigators.
tion. J Am Coll Cardiol 2006;47:76–84.
Influence of ejection fraction on cardiovascular outcomes in a broad
13. Liao L, Jollis JG, Anstrom KJ, Whellan DJ, Kitzman DW, Aurigemma GP,
spectrum of heart failure patients. Circulation 2005;112:3738–3744.
Mark DB, Schulman KA, Gottdiener JS. Costs for heart failure with
34. Burlew BS, Weber KT. Cardiac fibrosis as a cause of diastolic dysfunction.
normal vs reduced ejection fraction. Arch Intern Med 2006;166:
35. Schellings MW, Pinto YM, Heymans S. Matricellular proteins in the heart:
14. Bhatia RS, Tu JV, Lee DS, Austin PC, Fang J, Haouzi A, Gong Y, Liu PP.
possible role during stress and remodeling. Cardiovasc Res 2004;64:
Outcome of heart failure with preserved ejection fraction in a
population-based study. N Engl J Med 2006;355:260–269.
36. Sanderson JE. Heart failure with a normal ejection fraction. Heart 2007;
15. Aurigemma P. Diastolic heart failure—a common and lethal condition by
any name. N Engl J Med 2006;355:308–310.
37. Yusuf S, Pfeffer MA, Swedberg K, Granger CB, Held P, McMurray JJ,
16. Fischer M, Baessler A, Hense HW, Hengstenberg C, Muscholl M, Holmer S,
Michelson EL, Olofsson B, Ostergren J; CHARM Investigators Commit-
Doring A, Broeckel U, Riegger G, Schunkert H. Prevalence of left ventri-
tees. Effects of candesartan in patients with chronic heart failure and
cular diastolic dysfunction in the community: results from a Doppler
preserved left-ventricular ejection fraction: the CHARM-Preserved
echocardiographic-based survey of a population sample. Eur Heart J
Trial. Lancet 2003;362:777–781.
38. Maurer MS, El Khoury Rumberger L, King DL. Ventricular volume and
17. Klapholz M, Maurer M, Lowe AM, Messineo F, Meisner JS, Mitchell J,
length in hypertensive diastolic heart failure. J Am Soc Echocardiogr
Kalman J, Phillips RA, Steingart R, Brown EJ Jr, Berkowitz R,
Moskowitz R, Soni A, Mancini D, Bijou R, Sehhat K, Varshneya N,
39. Rame JE, Ramilo M, Spencer N, Blewett C, Mehta SK, Dries DL,
Kukin M, Katz SD, Sleeper LA, Le Jemtel TH; New York Heart Failure Con-
Drazner MH. Development of a depressed left ventricular ejection frac-
sortium. Hospitalization for heart failure in the presence of a normal
tion in patients with left ventricular hypertrophy and a normal ejection
left ventricular ejection fraction: results of the New York Heart
fraction. Am J Cardiol 2004;93:234–237.
Failure Registry. J Am Coll Cardiol 2004;43:1432–1438.
40. Drazner MH, Rame JE, Marino EK, Gottdiener JS, Kitzman DW,
18. Ferrari R, and the PREAMI Investigators. Effects of angiotensin-
Gardin JM, Manolio TA, Dries DL, Siscovick DS. Increased left ventricular
converting enzyme inhibition with perindopril on left ventricular remo-
mass is a risk factor for the development of a depressed left ventricular
deling and clinical outcome: results of the randomized Perindopril and
ejection fraction within five years. J Am Coll Cardiol 2004;43:
Remodeling in Elderly with Acute Myocardial Infarction (PREAMI)
Study. Arch Intern Med 2006;166:659–666.
41. Rosen BD, Edvardsen T, Lai S, Castillo E, Pan L, Herold MJ, Sinsha S,
19. Zile MR, Baicu CF, Gaasch WH. Diastolic heart failure—abnormalities in
Kronmal R, Arnett D, Crouse JR III, Heckbert SR, Bluemke DA,
active relaxation and passive stiffness of the left ventricle. N Engl J
Lima JAC. Left ventricular concentric remodeling is associated with
decreased global and regional systolic function. Circulation 2005;112:
20. Skaluba SJ, Litwin SE. Mechanisms of exercise intolerance. Insights from
Tissue Doppler Imaging. Circulation 2004;109:972–977.
42. Drazner MH. The transition from hypertrophy to failure. How certain are
21. Hadano Y, Murata K, Yamamoto T, Kunichika H, Matsumoto T, Akagawa E,
we? Circulation 2005;112:936–938.
Sato T, Tanaka T, Nose Y, Tanaka N, Matsuzaki M. Usefulness of mitral
43. Brockington IF, Edington GM, Olsen EG. Nigerian ‘heart muscle disease':
annular velocity in predicting exercise tolerance in patients with
the late stages of untreated hypertensive heart failure? Acta Cardiol
impaired left ventricular systolic function. Am J Cardiol 2006;97:
44. Sliwa K, Damasceno A, Mayosi BM. Epidemiology and etiology of cardio-
22. Baicu CF, Zile MR, Aurigemma GP, Gaasch WH. Left ventricular systolic
myopathy in Africa. Circulation 2005;112:3577–3583.
performance, function, and contractility in patients with diastolic
45. Kingue S, Dzudie A, Menanga A, Akono M, Ouankou M, Muna W. A new
heart failure. Circulation 2005;111:2306–2312.
look at adult chronic heart failure in Africa in the age of the Doppler
23. Yu CM, Lin H, Yang H, Kong SL, Zhang Q, Lee SWL. Progression of systolic
echocardiography: experience of the medicine department at Yaounde
abnormalities in patients with ‘isolated' diastolic heart failure and dias-
General Hospital. Ann Cardiol Angeiol (Paris) 2005;54:276–283.
tolic dysfunction. Circulation 2002;105:1195–1201.
46. Sanderson JE, Chan SK, Chan WW, Hung YT, Woo KS. The aetiology of
24. Yip G, Wang M, Zhang Y, Fung JW, Ho PY, Sanderson JE. Left ventricular
heart failure in the Chinese population of Hong Kong—a prospective
long axis function in diastolic heart failure is reduced in both diastole
study of 730 consecutive patients. Int J Cardiol 1995;51:29–35.
and systole: time for a redefinition? Heart 2002;87:121–125.
47. Nicholls MG, Richards AM. Is hypertension a leading cause of heart
25. Nikitin NP, Witte KK, Clark AL, Cleland JG. Color tissue Doppler-derived
failure in Chinese? Clin Exp Pharmacol Physiol 2002;29:850–851.
long-axis left ventricular function in heart failure with preserved global
48. Harris KM, Spirito P, Maron MS, Zenovich AG, Formisano F, Lesser JR,
systolic function. Am J Cardiol 2002;90:1174–1177.
Mackey-Bojack S, Manning WJ, Udelson JE, Maron BJ. Prevalence,
26. Petrie MC, Caruana L, Berry C, McMurray JJ. ‘Diastolic heart failure' or
clinical profile, and significance of left ventricular remodeling in the
heart failure caused by subtle left ventricular systolic dysfunction?
end-stage phase of hypertrophic cardiomyopathy. Circulation 2006;
27. Bruch C, Gradaus R, Gunia S, Breithardt G, Wichter T. Doppler tissue
49. Cahill JM, Ryan E, Travers B, Ryder M, Ledwidge M, McDonald K.
analysis of mitral annular velocities: evidence for systolic abnormalities
Progression of preserved systolic function heart failure to systolic
in patients with diastolic heart failure. J Am Soc Echocardiogr 2003;16:
dysfunction—a natural history study. Int J Cardiol 2006;106:95–102.
50. Douglas PS, Katz SE, Weinberg EO, Chen MH, Bishop SP, Lorell BH. Hyper-
28. Vinereanu D, Nicolaides E, Tweddel AC, Fraser AG. ‘Pure' diastolic dys-
trophic remodeling: gender differences in the early response to left
function is associated with long-axis systolic dysfunction. Implications
ventricular pressure overload. J Am Coll Cardiol 1998;32:1118–1125.
W.J. Paulus et al.
51. Wisloff U, Loennechen JP, Currie S, Smith GL, Ellingsen O. Aerobic exer-
cise reduces cardiomyocyte hypertrophy and increases contractility,
pressure-overloaded human heart. Circulation 2005;112:1136–1144.
Ca2þ sensitivity and SERCA-2 in rat after myocardial infarction.
72. Spinale FG, Coker ML, Heung LJ, Bond BR, Gunasinghe HR, Etoh T,
Cardiovasc Res 2002;54:162–174.
Goldberg AT, Zellner JL, Crumbley. A matrix metalloproteinase induc-
52. Jones JV, Raine AE, Sanderson JE, Carretta R, Graham DI. Adverse effect
tion/activation system exists in the human left ventricular myocardium
of chronic alcohol ingestion on cardiac performance in spontaneously
and is upregulated in heart failure. Circulation 2000;102:1944–1949.
hypertensive rats. J Hypertens 1988;6:419–422.
73. Polyakova V, Hein S, Kostin S, Ziegelhoeffer T, Schaper J. Matrix metal-
53. De Acetis M, Notte A, Accornero F, Selvetella G, Brancaccio M,
loproteinases and their tissue inhibitors in pressure-overloaded human
Vecchione C, Sbroggio M, Collino F, Pacchioni B, Lanfranchi G,
myocardium during heart failure progression. J Am Coll Cardiol 2004;
Aretini A, Ferretti R, Maffei A, Altruda F, Silengo L, Tarone G, Lembo G.
Cardiac overexpression of melusin protects from dilated cardiomyopathy
74. Hein S, Arnon E, Kostin S, Schonburg M, Elsasser A, Polyakova V,
due to long-standing pressure overload. Circ Res 2005;96:1087–1094.
Bauer EP, Klovekorn WP, Schaper J. Progression from compensated
54. Solomon SD, St John Sutton M, Lamas GA, Plappert T, Rouleau JL,
hypertrophy to failure in the pressure-overloaded human heart. Circula-
Skali H, Moye L, Braunwald E, Pfeffer MA, Survival Ventricular Enlarge-
ment (SAVE) Investigators. Ventricular remodeling does not accompany
75. Hasenfuss G, Pieske B. Calcium cycling in congestive heart failure. J Mol
the development of heart failure in diabetic patients after myocardial
Cell Cardiol 2002;34:951–969.
76. Beuckelmann DJ, Nabauer M, Erdmann E. Intracellular calcium handling
55. Tenenbaum A, Fisman EZ, Schwammenthal E, Adler Y, Benderly M,
in isolated ventricular myocytes from patients with terminal heart
Motro M, Shemesh J. Increased prevalence of left ventricular hypertro-
failure. Circulation 1992;85:1046–1055.
phy in hypertensive women with type 2 diabetes mellitus. Cardiovasc
77. Schmidt U, Hajjar RJ, Helm PA, Kim CS, Doye AA, Gwathmey JK. Contri-
Diabetol 2003;2:14.
bution of abnormal sarcoplasmic reticulum ATPase activity to systolic
56. Katz AM, Zile MR. New molecular mechanisms in diastolic heart failure.
and diastolic dysfunction in human heart failure. J Mol Cell Cardiol
57. Gerdes AM. Cardiac myocyte remodeling in hypertrophy and progression
78. Schmidt U, del Monte F, Miyamoto MI, Matsui T, Gwathmey JK,
to failure. J Card Fail 2002;8:S264–S268.
Rosenzweig A, Hajjar RJ. Restoration of diastolic function in senescent
58. Kitzman DW, Little WC, Brubaker PH, Anderson RT, Hundley WG,
rat hearts through adenoviral gene transfer of sarcoplasmic reticulum
Marburger CT, Brosnihan B, Morgan TM, Stewart KP. Pathophysiological
characterization of isolated diastolic heart failure in comparison to
79. Pieske B, Maier LS, Piacentino V III, Weisser J, Hasenfuss G, Houser S.
systolic heart failure. JAMA 2002;288:2144–2150.
Rate dependence of [Naþ]i and contractility in nonfailing and failing
59. Brucks S, Little WC, Chao T, Kitzman DW, Wesley-Farrington D, Gandhi S,
human myocardium. Circulation 2002;106:447–453.
Shihabi ZK. Contribution of left ventricular diastolic dysfunction to heart
80. Hasenfuss G, Schillinger W, Lehnart SE, Preuss M, Pieske B, Maier LS,
failure regardless of ejection fraction. Am J Cardiol 2005;95:603–606.
Prestle J, Minami K, Just H. Relationship between Naþ-Ca2þ-exchanger
60. Zile MR, Gaasch WH, Carroll JD, Feldman MD, Aurigemma GP, Schaer GL,
protein levels and diastolic function of failing human myocardium. Cir-
Ghali JK, Liebson PR. Heart failure with a normal ejection fraction: is
measurement of diastolic function necessary to make the diagnosis of
81. Pieske B, Houser SR. [Naþ] i handling in the failing human heart. Cardi-
diastolic heart failure? Circulation 2001;104:779–782.
ovasc Res 2003;57:874–876.
61. Van Heerebeek L, Borbely A, Niessen HW, Bronzwaer JGF, van der
82. Cleland JG, Tendera M, Adamus J, Freemantle N, Polonski L, Taylor J.
Velden J, Stienen GJ, Linke WA, Laarman GJ, Paulus WJ. Myocardial
The perindopril in elderly people with chronic heart failure (PEP-CHF)
structure and function differ in systolic and diastolic heart failure.
study. Eur Heart J 2006;27:2338–2345.
83. Swedberg K, Cleland J, Dargie H, Drexler H, Follath F, Komajda M,
´ly A, van der Velden J, Papp Z, Bronzwaer JGF, Edes I, Stienen GJ,
Tavazzi L, Smiseth OA, Gavazzi A, Haverich A, Hoes A, Jaarsma T,
Paulus WJ. Cardiomyocyte stiffness in diastolic heart failure. Circula-
Korewicki J, Levy S, Linde C, Lopez-Sendon JL, Nieminen MS,
Pierard L, Remme WJ; Task Force for the Diagnosis and Treatment of
63. Neagoe C, Opitz CA, Makarenko I, Linke WA. Gigantic variety: expression
Chronic Heart Failure of the European Society of Cardiology. Guidelines
patterns of titin isoforms in striated muscles and consequences for myo-
for the diagnosis and treatment of chronic heart failure: executive
fibrillar passive stiffness. J Muscle Res Cell Mot 2003;24:175–189.
summary (update 2005): The Task Force for the Diagnosis and Treatment
64. Yotti R, Bermejo J, Antoranz JC, Desco MM, Cortina C, Rojo-Alvarez JL,
of Chronic Heart Failure of the European Society of Cardiology. Eur
Allue C, Martin L, Moreno M, Serrano JA, Munoz R, Garcia-Fernandez MA.
Heart J 2005;26:1115–1140.
A noninvasive method for assessing impaired diastolic suction in patients
84. Packer M. Abnormalities of diastolic function as potential cause of exer-
with dilated cardiomyopathy. Circulation 2005;112:2921–2929.
cise intolerance in chronic heart failure. Circulation 1990;81:III-78–86.
65. Lim CC, Sawyer DB. Modulation of cardiac function: titin springs into
85. Mancini DM, Eisen H, Kussmaul W, Mull R, Edmunds LH Jr, Wilson JR.
action. J Gen Physiol 2005;125:249–252.
Value of peak exercise oxygen consumption for optimal timing of
66. Fukuda N, Wu Y, Nair P, Granzier HL. Phosphorylation of titin modulates
cardiac transplantation in ambulatory patients with heart failure.
passive stiffness of cardiac muscle in a titin isoform-dependent manner.
J Gen Physiol 2005;125:257–271.
86. Weber K, Kinasewitz G, Janicki J, Fishman A. Oxygen utilisation and
67. Makarenko I, Opitz CA, Leake MC, Kulke M, Gwathmey JK, del Monte F,
ventilation during exercise in patients with chronic cardiac failure.
Hajjar RJ, Linke WA. Passive stiffness changes caused by upregulation of
compliant titin isoforms in human dilated cardiomyopathy hearts. Circ
87. Cohen-Solal A, Laperche T, Morvan D, Geneves M, Caviezel B,
Gourgon R. Prolonged kinetics of recovery of oxygen consumption
68. Nagueh SF, Shah G, Wu Y, Torre-Amione G, King NM, Lahmers S, Witt CC,
after maximal graded exercise in patients with chronic heart failure.
Becker K, Labeit S, Granzier HL. Altered titin expression, myocardial
stiffness, and left ventricular function in patients with dilated cardio-
88. Pardaens K, Vanhaecke J, Fagard RH. Impact of age and gender on peak
myopathy. Circulation 2004;110:155–162.
oxygen uptake in chronic heart failure. Med Sci Sports Exerc 1997;29:
69. Neagoe C, Kulke M, del Monte F, Gwathmey JK, de Tombe PP, Hajjar RJ,
Linke WA. Titin isoform switch in ischaemic human heart disease.
89. Working Group on Cardiac Rehabilitation & Exercise Physiology and
Working Group on Heart Failure of the European Society of Cardiology.
70. Ahmed SH, Clark LL, Pennington WR, Webb CS, Bonnema DD,
Recommendations for exercise testing in chronic heart failure patients.
Leonardi AH, McClure CD, Spinale FG, Zile MR. Matrix metalloprotei-
Eur Heart J 2001;22:37–45.
nases/tissue inhibitors of metalloproteinases. Relationship between
90. Bittner V, Weiner DH, Yusuf S, Rogers WJ, McIntyre KM, Bangdiwala SI,
changes in proteolytic determinants of matrix composition and struc-
Kronenberg MW, Kostis JB, Kohn RM, Guillotte M. Prediction of mortality
tural, functional, and clinical manifestations of hypertensive heart
and morbidity with a 6 min walk test in patients with left ventricular
disease. Circulation 2006;113:2089–2096.
dysfunction. SOLVD Investigators. JAMA 1993;270:1702–1707.
71. Heymans S, Schroen B, Vermeersch P, Milting H, Gao F, Kassner A,
91. Opasich C, Pinna GD, Mazza A, Febo O, Riccardi PG, Capomolla S,
Gillijns H, Herijgers P, Flameng W, Carmeliet P, Van de Werf F,
Cobelli F, Tavazzi L. Reproducibility of the sixminute walking test in
Pinto YM, Janssens S. Increased cardiac expression of tissue inhibitor
patients with chronic congestive heart failure: practical implications.
of metalloproteinase-1 and tissue inhibitor of metalloproteinase-2 is
Am J Cardiol 1998;81:1497–1500.
How to diagnose diastolic heart failure
92. Cahalin LP, Mathier MA, Semigran MJ, Dec GW, DiSalvo TG. The six-
117. Mottram PM, Leano R, Marwick TH. Usefulness of B-type natriuretic
minute walk test predicts peak oxygen uptake and survival in patients
peptide in hypertensive patients with exertional dyspnea and normal
with advanced heart failure. Chest 1996;110:325–332.
left ventricular ejection fraction and correlation with new echocardio-
93. Vasan RS, Levy D. Defining diastolic heart failure: a call for standardized
graphic indexes of systolic and diastolic function. Am J Cardiol 2003;92:
diagnostic criteria. Circulation 2000;101:2118–2121.
94. Yturralde RF, Gaasch WH. Diagnostic criteria for diastolic heart failure.
118. Vasan RS, Benjamin EJ. Diastolic heart failure—no time to relax. N Engl J
Prog Cardiovasc Dis 2005;47:314–319.
95. Lang RM, Bierig M, Devereux RB, Flachskampf FA, Foster E, Pellikka PA,
119. Badano LP, Albanese De Biaggio P, Rozbowsky P, Miani D, Fresco C,
Picard MH, Roman MJ, Seward J, Shamewise J, Solomon S, Spencer KT,
Fioretti PM. Prevalence, clinical characteristics, quality of life, and
St John Sutton M, Stewart W. Recommendations for chamber quantifi-
prognosis of patients with congestive heart failure and isolated left ven-
cation. Eur J Echocardiography 2006;7:79–108.
tricular diastolic dysfunction. J Am Soc Echocardiogr 2004;17:253–261.
96. Brutsaert DL, Sys SU. Relaxation and diastole of the heart. Physiol Rev
120. Rusconi C, Sabatini T, Faggiano P, Ghizzoni G, Oneglia C, Simoncelli U,
Gualeni A, Sorgato A, Marchetti A. Prevalence of isolated left ventri-
97. Gaasch WH, Blaustein AS, Andrias CW, Donahue RP, Avitall B. Myocardial
cular diastolic dysfunction in hypertension as assessed by combined
relaxation II: hemodynamic determinants of rate of left ventricular iso-
transmitral and pulmonary vein flow Doppler study. Am J Cardiol
volumic pressure decline. Am J Physiol 1980;239:H1–H6.
98. Raff GL, Glantz SA. Volume loading slows left ventricular isovolumic
121. Rossvoll O, Hatle LK. Pulmonary venous flow velocities recorded by
relaxation rate. Evidence of load-dependent relaxation in the intact
transthoracic Doppler ultrasound: relation to left ventricular diastolic
dog heart. Circ Res 1981;48:813–824.
pressures. J Am Coll Cardiol 1993;21:1687–1696.
99. Leite-Moreira AF, Gillebert TC. Nonuniform course of left ventricular
122. Yamamoto K, Nishimura RA, Burnett JC Jr, Redfield MM. Assessment of
pressure fall and its regulation by load and contractile state. Circulation
left ventricular end-diastolic pressure by Doppler echocardiography:
contribution of duration of pulmonary venous versus mitral flow velocity
100. Leite-Moreira AF, Correia-Pinto J. Load as an acute determinant of end-
curves at atrial contraction. J Am Soc Echocardiogr 1997;10:52–59.
diastolic pressure-volume relation. Am J Physiol Heart Circ Physiol
123. Jensen JL, Williams FE, Beilby BJ, Johnson BL, Miller LK, Ginter TL,
Tomaselli-Martin G, Appleton CP. Feasibility of obtaining pulmonary
101. Kass DA, Bronzwaer JGF, Paulus WJ. What Mechanisms Underlie Diastolic
venous flow velocity in cardiac patients using transthoracic pulsed
Dysfunction in Heart Failure? Circ Res 2004;94:1533–1542.
wave Doppler technique. J Am Soc Echocardiogr 1997;10:60–66.
102. Gandhi SK, Powers JC, Nomeir AM, Fowle K, Kitzman DW, Rankin KM,
124. Rocca HP, Rickli H, Attenhofer Jost CH, Jenni R. Left ventricular end-
Little WC. The pathogenesis of acute pulmonary edema associated
diastolic pressure can be estimated by either changes in transmitral
with hypertension. N Engl J Med 2001;344:17–22.
inflow pattern during valsalva maneuver or analysis of pulmonary
103. Hirota Y. A clinical study of left ventricular relaxation. Circulation 1980;
venous flow. J Am Soc Echocardiogr 2000;13:599–607.
125. O'Leary PW, Durongpisitkul K, Cordes TM, Bailey KR, Hagler DJ, Tajik J,
104. Paulus WJ, Bronzwaer JGF, Felice H, Kishan N, Wellens F. Deficient
Seward JB. Diastolic ventricular function in children: a Doppler echocar-
acceleration of left ventricular relaxation during exercise after heart
diographic study establishing normal values and predictors of increased
ventricular end-diastolic pressure. Mayo Clin Proc 1998;73:616–628.
105. Yamakado T, Takagi E, Okubo S, Imanaka-Yoshida K, Tarumi T,
126. Appleton CP, Firstenberg MS, Garcia MJ, Thomas JD. The echo-Doppler
Nakamura M, Nakano T. Effects of aging on left ventricular relaxation
evaluation of left ventricular diastolic function. A current perspective.
in humans. Circulation 1997;95:917–923.
Cardiol Clin 2000;18:513–546. ix.
106. Little WC, Downes TR. Clinical evaluation of left ventricular diastolic
127. Kimura K, Murata K, Tanaka N, Ueda K, Wada Y, Liu J, Ohyama R, Fujii T,
performance. Prog Cardiovasc Dis 1990;32:273–290.
Matsuzaki M. The importance of pulmonary venous flow measurement
107. Grossman W. Relaxation and diastolic distensibility of the regionally
for evaluating left ventricular end-diastolic pressure in patients with
ischaemic left ventricle. In: Grossman W, Lorell BH, eds. Diastolic Relax-
coronary artery disease in the early stage of diastolic dysfunction.
ation of the Heart. Boston: Martinus Nijhoff; 1987. p193–203.
J Am Soc Echocardiogr 2001;14:987–993.
108. Paulus WJ, Shah AM. NO and cardiac diastolic function. Cardiovasc Res
128. Rossi A, Loredana L, Cicoira M, Bonapace S, Zanolla L, Zardini P, Golia G.
Additional value of pulmonary vein parameters in defining pseudonor-
109. Leite-Moreira AF, Bras-Silva C, Pedrosa CA, Rocha-Sousa AA. ET-1
malization of mitral inflow pattern. Echocardiography 2001;18:
increases distensibility of acutely loaded myocardium: a novel ETA
and Naþ/Hþ exchanger-mediated effect. Am J Physiol Heart Circ
129. Paraskevaidis IA, Tsiapras DP, Karavolias GK, Cokkinos P, Kremastinos DT.
Doppler-derived left ventricular end-diastolic pressure prediction model
110. Leite-Moreira AF, Castro-Chaves P, Pimentel-Nunes P, Lima-Carneiro A,
using the combined analysis of mitral and pulmonary A waves in patients
Guerra MS, Soares JB, Ferreira-Martins J. Angiotensin II acutely
with coronary artery disease and preserved left ventricular systolic
decreases myocardial stiffness: a novel AT1, PKC and Naþ/Hþ
function. Am J Cardiol 2002;90:720–724.
exchanger-mediated effect. Br J Pharmacol 2006;147:690–697.
130. Yamada H, Goh PP, Sun JP, Odabashian J, Garcia MJ, Thomas JD,
111. Caruana L, Davie AP, Petrie M, McMurray J. Diagnosing heart failure. Eur
Klein AL. Prevalence of left ventricular diastolic dysfunction by
Heart J 1999;20:393.
Doppler echocardiography: clinical application of the Canadian consen-
112. Palmieri V, Innocenti F, Pini R, Celentano A. Reproducibility of Doppler
sus guidelines. J Am Soc Echocardiogr 2002;15:1238–1244.
echocardiographic assessment of left ventricular diastolic function in
131. Hadano Y, Murata K, Liu J, Oyama R, Harada N, Okuda S, Hamada Y,
multicenter setting. J Am Soc Echiocardiogr 2005;18:99–106.
Tanaka N, Matsuzaki M. Can transthoracic Doppler echocardiography
113. Cahill John M, Horan Mairead, Quigley Peter, Maurer Brian J, McDonald
predict the discrepancy between left ventricular end-diastolic pressure
Ken. Doppler-echocardiographic indices of diastolic function in heart
and mean pulmonary capillary wedge pressure in patients with heart
failure admissions with preserved left ventricular systolic function.
failure? Circ J 2005;69:432–438.
Eur J Heart Fail 2002;4:473–478.
132. Dini FL, Michelassi C, Micheli G, Rovai D. Prognostic value of pulmonary
114. Thomas MD, Fox KF, Wood DA, Gibbs JS, Coats AJ, Henein MY,
venous flow Doppler signal in left ventricular dysfunction: contribution
Poole-Wilson PA, Sutton GC. Echocardiographic features and brain
of the difference in duration of pulmonary venous and mitral flow at
natriuretic peptides in patients presenting with heart failure and
atrial contraction. J Am Coll Cardiol 2000;36:1295–1302.
preserved systolic function. Heart 2006;92:603–608.
133. Rivas-Gotz C, Khoury DS, Manolios M, Rao L, Kopelen HA, Nagueh SF.
115. Petrie MC, Hogg K, Caruana L, Mc Murray JJV. Poor concordance of com-
Time interval between onset of mitral inflow and onset of early diastolic
monly used echocardiographic measures of left ventricular diastolic
velocity by tissue Doppler: a novel index of left ventricular relaxation:
function in patients with suspected heart failure but preserved systolic
experimental studies and clinical application. J Am Coll Cardiol 2003;
function: is there a reliable echocardiographic measure of diastolic
dysfunction? Heart 2004;90:511–517.
134. Diwan A, McCulloch M, Lawrie GM, Reardon MJ, Nagueh SF. Doppler esti-
116. Lim T, Ashrafian H, Dwivedi G, Collinson P, Senior R. Increased left atrial
mation of left ventricular filling pressures in patients with mitral valve
volume index is an independent predictor of raised serum natriuretic
disease. Circulation 2005;111:3281–3289.
peptide in patients with suspected heart failure but normal left ventri-
135. Ommen SR, Nishimura RA, Appleton CP, Miller FA, Oh JK, Redfield MM,
cular ejection fraction: Implication for diagnosis of diastolic heart
failure. Eur J Heart Fail 2006;8:38–45.
tissue Doppler imaging in the estimation of left ventricular filling
W.J. Paulus et al.
pressures: A comparative simultaneous Doppler-catheterization study.
150. McDonagh TA, Holmer S, Raymond I, Luchner A, Hildebrant P, Dargie HJ.
NT-proBNP and the diagnosis of heart failure: a pooled analysis of three
136. Hillis GS, Moller JE, Pellikka PA, Gersh BJ, Wright RS, Ommen SR,
European epidemiological studies. Eur J Heart Failure 2004;6:269–273.
Reeder GS, Oh JK. Noninvasive estimation of left ventricular filling
151. Jones AE, Kline JA. Elevated brain natriuretic peptide in septic patients
pressure by E/e0 is a powerful predictor of survival after acute myocar-
without heart failure. Ann Emerg Med 2003;42:714–715.
dial infarction. J Am Coll Cardiol 2004;43:360–367.
152. La Villa G, Romanelli RG, Casini Raggi V, Tosti-Guerra C, De Feo ML,
137. Dokainish H, Zoghbi WA, Lakkis NM, Al-Bakshy F, Dhir M, Quinones MA,
Marra F, Laffi G, Gentilini P. Plasma levels of brain natriuretic peptide
Nagueh SF. Optimal noninvasive assessment of left ventricular filling
in patients with cirrhosis. Hepatology 1992;16:156–161.
pressures: a comparison of tissue Doppler echocardiography and
153. Forfia PR, Watkins SP, Rame JE, Stewart KJ, Shapiro EP. Relationship
B-type natriuretic peptide in patients with pulmonary artery catheters.
between B-type natriuretic peptides and pulmonary capillary wedge
pressure in the intensive care unit. J Am Coll Cardiol 2005;45:
138. Nagueh SF, Middleton KJ, Kopelen HA, Zoghbi WA, Quinones MA. Doppler
tissue imaging: a noninvasive technique for evaluation of left ventricu-
154. Tsutamoto T, Wada A, Sakai H, Ishikawa C, Tanaka T, Hayashi M, Fujii M,
lar relaxation and estimation of filling pressures. J Am Coll Cardiol 1997;
Yamamoto T, Dohke T, Ohnishi M, Takashima H, Kinoshita M, Horie M.
Relationship between renal function and plasma brain natriuretic
139. Edvardsen T, Gerber BL, Garot J, Bluemke DA, Lima JA, Smiseth OA.
peptide in patients with heart failure. J Am Coll Cardiol 2006;47:
Quantitative assessment of intrinsic regional myocardial deformation
by Doppler strain rate echocardiography in humans: validation against
155. Ando T, Ogawa K, Yamaki K, Hara M, Takagi K. Plasma concentrations of
three-dimensional tagged magnetic resonance imaging. Circulation
atrial, brain, and C-type natriuretic peptides and endothelin-1 in
patients with chronic respiratory diseases. Chest 1996;110:462–468.
140. Tsang TS, Barnes ME, Gersh BJ, Takemoto Y, Rosales AG, Bailey KR,
156. TulevskiII, Hirsch A, Sanson BJ, Romkes H, van der Wall EE, van
Veldhuisen DJ, Buller HR, Mulder BJ. Increased brain natriuretic
Seward JB. Prediction of risk for first age-related cardiovascular
peptide as a marker for right ventricular dysfunction in acute pulmonary
events in an elderly population: the incremental value of echocardio-
embolism. Thromb Haemost 2001;86:1193–1196.
graphy. J Am Coll Cardiol 2003;42:1199–1205.
157. Thorens JB, Ritz M, Reynard C, Righetti A, Vallotton M, Favre H, Kyle U,
141. Pritchett AM, Mahoney DW, Jacobsen SJ, Rodeheffer RJ, Karon BL,
Jolliet P, Chevrolet JC. Haemodynamic and endocrinological effects of
Redfield MM. Diastolic dysfunction and left atrial volume: a population-
noninvasive mechanical ventilation in respiratory failure. Eur Respir J
based study. J Am Coll Cardiol 2005;45:87–92.
142. Douglas PS. The left atrium: a biomarker of chronic diastolic dysfunction
158. Horwich TB, Hamilton MA, Fonarow GC. B-type natriuretic peptide
and cardiovascular disease risk. J Am Coll Cardiol 2003;42:1206–1207.
levels in obese patients with advanced heart failure. J Am Coll
143. Alsaileek AA, Osranek M, Fatema K, McCully RB, Tsang TS, Seward JB.
Predictive value of normal left atrial volume in stress echocardiography.
159. Daniels LB, Clopton P, Bhalla V, Krishnaswamy P, Nowak RM, McCord J,
J Am Coll Cardiol 2006;47:1024–1028.
Hollander JE, Duc P, Omland T, Storrow AB, Abraham WT, Wu AH,
144. Tsang TS, Barnes ME, Gersh BJ, Bailey KR, Seward JB. Left atrial volume
as a morphological expression of left ventricular diastolic dysfunction
Herrmann HC, McCullough PA, Maisel AS. How obesity affects the cut-
and relation to cardiovascular risk burden. Am J Cardiol 2002;90:
points for B-type natriuretic peptide in the diagnosis of acute heart
failure. Results from the Breathing Not Properly Multinational Study.
145. Tsang TS, Abhayaratna WP, Barnes ME, Miyasaka Y, Gersh BJ, Bailey KR,
Am Heart J 2006;151:999–1005.
Cha SS, Seward JB. Prediction of cardiovascular outcomes with left
160. Maisel AS, McCord J, Nowak RM, Hollander JE, Wu AH, Duc P, Omland T,
atrial size: is volume superior to area or diameter? J Am Coll Cardiol
Storrow AB, Krishnaswamy P, Abraham WT, Clopton P, Steg PG,
146. Tschope C, Kasner M, Westermann D, Gaub R, Poller WC, Schultheiss HP.
Kazanegra R, Herrmann HC, McCullough PA; Breathing Not Properly Mul-
The role of NT-proBNP in the diagnostics of isolated diastolic dysfunc-
tinational Study Investigators. Bedside B-type natriuretic peptide in the
tion: correlation with echocardiographic and invasive measurements.
emergency diagnosis of heart failure with reduced or preserved ejection
Eur Heart J 2005;26:2277–2284.
fraction. J Am Coll Cardiol 2003;41:2010–2017.
147. Watanabe S, Shite J, Takaoka H, Shinke T, Imuro Y, Ozawa T, Otake H,
161. Rademakers FE. Magnetic resonance imaging in cardiology. Lancet 2003;
Matsumoto D, Ogasawara D, Paredes OL, Yokoyama M. Myocardial stiff-
ness is an important determinant of the plasma brain natriuretic
162. Hauser TH, McClennen S, Katsimaglis G, Josephson ME, Manning WJ,
peptide concentration in patients with both diastolic and systolic
Yeon SB. Assessment of left atrial volume by contrast enhanced mag-
heart failure. Eur Heart J 2006;27:832–838.
netic resonance angiography. J Cardiovasc Magn Reson 2004;6:491–497.
148. Lubien E, DeMaria A, Krishnaswamy P, Clopton P, Koon J, Kazanegra R,
163. Gotte MJ, Germans T, Russell IK, Zwanenburg JJ, Marcus JT, van
Gardetto N, Wanner E, Maisel AS. Utility of B-natriuretic peptide in
Rossum AC, van Veldhuisen DJ. Myocardial strain and torsion quantified
detecting diastolic dysfunction: comparison with Doppler velocity
by cardiovascular magnetic resonance tissue tagging studies in normal
recordings. Circulation 2002;105:595–601.
and impaired left ventricular function. J Am Coll Cardiol 2006;48:
149. Redfield MM, Rodeheffer RJ, Jacobsen SJ, Mahoney DW, Bailey KR,
Burnett JC Jr. Plasma brain natriuretic peptide to detect preclinical
164. Oh JK, Hatle L, Tajik AJ, Little WC. Diastolic heart failure can be diag-
ventricular systolic or diastolic dysfunction: a community-based study.
nosed by comprehensive two-dimensional and Doppler echocardiogra-
phy. J Am Coll Cardiol 2006;47:500–506.
Source: http://www.carsten-tschoepe.de/usr_files/6_Paper%2010.pdf
Buss-SMS-Canzler is a leading inter- More than 500 dryers national supplier of thermal separa- tion solutions for difficult products For more than 50 years we have sup- and mixtures. plied different types of dryers, adap- We are the world's leading supplier ted to a large variety of applications of thin film evaporation technology, throughout the world, currently more
nature publishing group state art Antiobesity Pharmacotherapy: New Drugs and Emerging TargetsGW Kim1, JE Lin1, ES Blomain1 and SA Waldman1 Obesity is a growing pandemic, and related health and economic costs are staggering. Pharmacotherapy, partnered with lifestyle modifications, forms the core of current strategies to reduce the burden of this disease and its sequelae. However, therapies targeting weight loss have a significant history of safety risks, including cardiovascular and psychiatric events. Here, evolving strategies for developing antiobesity therapies, including targets, mechanisms, and developmental status, are highlighted. Progress in this field is underscored by Belviq (lorcaserin) and Qsymia (phentermine/topiramate), the first agents in more than 10 years to achieve regulatory approval for chronic weight management in obese patients. On the horizon, novel insights into metabolism and energy homeostasis reveal guanosine 3′,5′-cyclic monophosphate (cGMP) signaling circuits as emerging targets for antiobesity pharmacotherapy. These innovations in molecular discovery may elegantly align with practical off-the-shelf approaches, leveraging existing approved drugs that modulate cGMP levels for the management of obesity.



