Everyvoicecounts.org
Crusted Scabies in
Remote Aboriginal
Communities2014 EDITIONChronic disease case management of crusted scabies
to break the cycle of recurrences and transmission
Document prepared by:
Program design and people empowerment
CRUSTED SCABIES AND ITS SIGNIFICANCE
A severe form of scabies, caused when an individual's immune system is not able to control mite
Hyper-infection develops, often with up to a million or more scabies mites. This is compared with 5-10
mites in simple scabies.
Abnormally thick layers of keratinised cells in the stratum corneum, mixed with thousands of scabies
mites, eggs, mite faeces and shed skin. Hyperkeratosis can be localised or widespread.
In scabies endemic areas, crusted scabies must be treated as a chronic condition.
What is its significance?
Individuals with crusted scabies experience lower life expectancy, frequent hospitalisations and develop
secondary bacterial complications.
Household contacts of unmanaged crusted scabies have high risk of recurrent scabies, Strep A skin sores,
poor sleep, disruption of school and work. Strep A skin sores are associated with chronic heart and renal disease.
Crusted scabies is highly infectious and causes outbreaks of scabies. Effective management is essential to the
control of scabies in communities.
*All clinical protocols in the guide are based on the CARPA Standard Treatment Manual 6th Ed. Please follow CARPA at all times
WHAT IS IT MANAGING CRUSTED SCABIES IN REMOTE ABORIGINAL COMMUNITIES 2014 EDITION 1
4. Chronic care plan
Aim is to reduce recurrences and
impact of disease on patient,
Contact One Disease to
add name to crusted
Confirm crusted scabies
Consult Infectious
Critical part of
Disease Team at Royal
(08 8922 8888) or
Alice Springs Hospital
Therapeutic rapport
and building capacity for
With senior member of
house. PAGE 14-16
Develop treatment
plan with patient, consult
Infectious Disease Team
SUMMARY OF GUIDE MANAGING CRUSTED SCABIES IN REMOTE ABORIGINAL COMMUNITIES 2014 EDITION 2
Diagnosis can be difficultPrompt and correct diagnoses of crusted scabies is vital. Misdiagnosis results in unnecessary and expensive treatment and puts the patient on an unnecessary chronic condition management plan. Time spent properly confirming diagnoses will save time and resources in the future.
To make a positive diagnosis you must confirm a & b, (and ideally c & d);
A Identify / confirm clinical appearanceB Skin scrapingsC Audit patient clinical filesD Contact tracing
1. DIAGNOSIS MANAGING CRUSTED SCABIES IN REMOTE ABORIGINAL COMMUNITIES 2014 EDITION 3
A Identify / confirm clinical appearance
Characteristic crusted skin patches;
Thickened, scaly skin patches. Often not itchy.
Often, but not always on buttocks, hands, feet, elbows, armpits Scale may have distinctive creamy colour Do not confuse with tinea, psoriasis, eczema or dermatitis as it may look similar.
Specialist diagnosis recommended;
The diagnosis can be difficult. Always consult Infectious Disease Team via switch at Royal Darwin Hospital 08
8922 8888 or Alice Springs Hospital 08 8951 7777.
As underlying immune deficiency can be cause of the disease further testing is warranted. Discuss with
infectious disease specialist.
Staff and carers should practice infection control procedures including wearing disposable gloves.
Take care not to come in contact with scabies-containing fomites such as bedding or seating.
If you think you have been exposed to scabies during the course of your work you may wish to apply a
scabicide cream preventatively (e.g. benzyl benzoate) to exposed areas.
1. DIAGNOSIS MANAGING CRUSTED SCABIES IN REMOTE ABORIGINAL COMMUNITIES 2014 EDITION 4
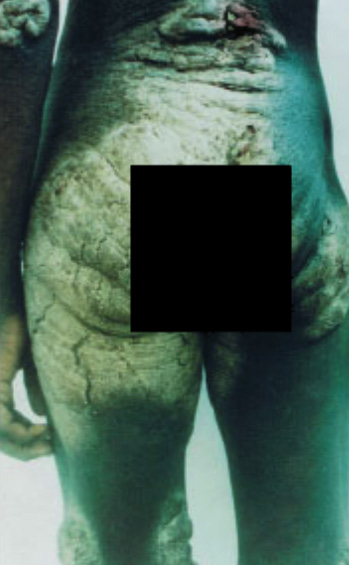

A Clinical appearance
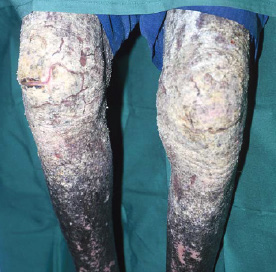
Hyper-keratotic (thick, scaly, cream coloured) areas with significant skin shedding (highly infectious).
Crusted Scabies cannot be
Depigmented areas of skin. This is evidence of repeated recurrences of past
excluded unless buttocks
crusting signifying chronicity and severity (add to grading scale pg 12).
are seen (common area for crusts).
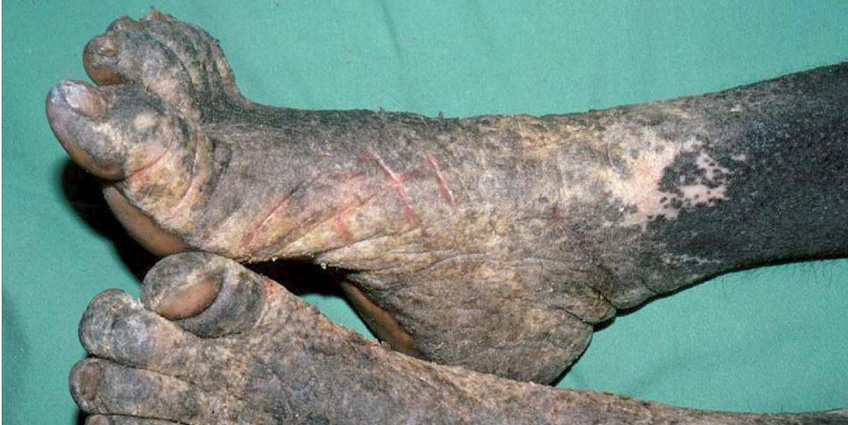
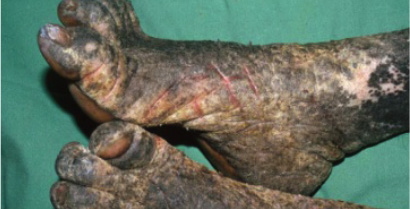
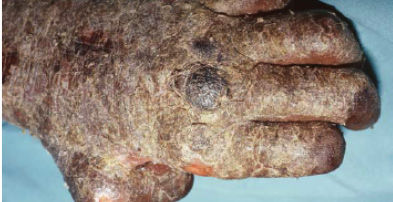
Crusted scabies in a patient with claw hand from
past leprosy.
Crusted scabies of the toes and feet.
1. DIAGNOSIS MANAGING CRUSTED SCABIES IN REMOTE ABORIGINAL COMMUNITIES 2014 EDITION 5
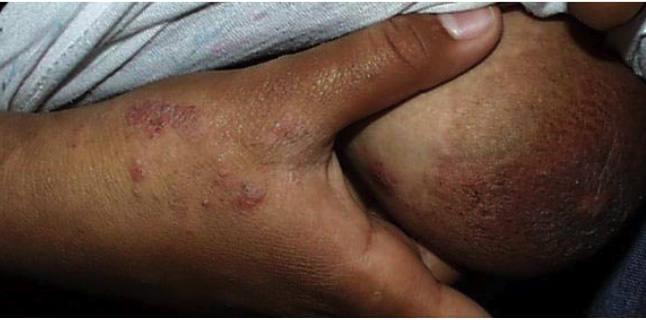
A Clinical Appearance: Common errors
* It is common for immediate contacts of patients with crusted scabies to be
misdiagnosed. See p9 for more information about contact tracing.
Misdiagnosing crusted sores (scabs, dry exudate) and or fungal as crusted scabies
Scabies papules.
Crusted sores and fungal.
This is not crusted scabies.
Scabies vesicle.
This is simple scabies with localised epidermal thickening.
This is not crusted scabies.
1. DIAGNOSIS MANAGING CRUSTED SCABIES IN REMOTE ABORIGINAL COMMUNITIES 2014 EDITION 6
1. Identify an area of suspected crusting (thickened, scaly skin).
2. Gently use the sharp side of a sterile scalpel held at a 90º angle to scrape loose flakes of skin into a sterile
urine collection jar. If true crusting is present skin should be easily collected.
Collect loose flakes of skin from areas of
Collection technique
suspected crusting
3. Don't rush the process. The more skin collected the greater the chance of confirming the diagnosis.
A few pieces of skin may be sufficient, but collect as much skin as possible.
4. If skin is not readily falling into the jar crusted scabies is less likely.
5. Do not cut or injure the skin. Infection and sepsis is a real risk in these patients.
6. Send collected sample to lab for testing. Make sure to request testing of scabies mites.
7. Absence of mites from skin scrapings does not rule out the possibility of crusted scabies. If results are
positive this greatly increases the likelihood of crusted scabies.
1. DIAGNOSIS MANAGING CRUSTED SCABIES IN REMOTE ABORIGINAL COMMUNITIES 2014 EDITION 7
C Audit patient clinical files
People who develop crusted scabies once are vulnerable to redeveloping the disease for life. They often
have multiple admissions for crusted scabies going back many years. With clinic staff turnover this knowledge can be lost.
Review electronic notes for past diagnoses and or hospitalisation for crusted scabies.
If available review paper notes for past diagnoses and or hospitalisation for crusted scabies.
Add past crusted scabies to grading scale pg 11.
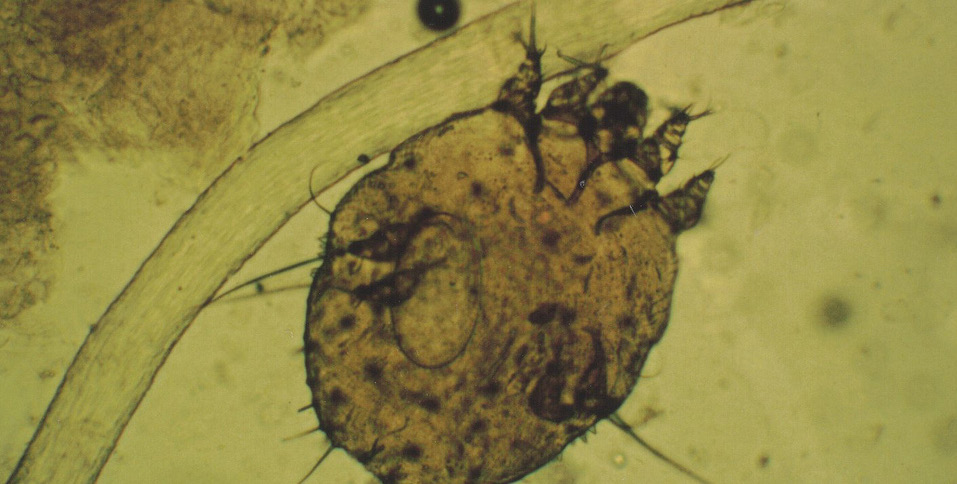
Magnified scabies mites.
1. DIAGNOSIS MANAGING CRUSTED SCABIES IN REMOTE ABORIGINAL COMMUNITIES 2014 EDITION 8
D Contact tracing
Crusted scabies patients are super spreaders/core transmitters of scabies. With outbreaks of scabies or recurrent scabies in families look for crusted scabies.
Close contacts of crusted scabies can exhibit severe scabies rashes and have been misdiagnosed with
crusted scabies (crusted scabies like condition).
Condition can mimic crusted scabies and may be positive for mites on scrapings.
If primary and secondary contacts have little to no scabies crusted scabies is unlikely.
Children with 10 or more interactions with the local health centre for scabies in a one year period
strongly indicate uncontrolled crusted scabies in their household.
Likely to share a bed/bedroom with
crusted scabies patient.
Primary contacts
Exposed to thousands of mites.
(crusted scabies
Condition can mimic crusted scabies
including high mite loads on scrapings.
Not true crusted scabies. May be
misdiagnosed as crusted scabies.
Live in or frequently visit same location
as crusted scabies patient.
Secondary contacts
Develops severe scabies and sores.
This is particularly true for young children in the house.
Infrequent contact with case.
Tertiary contacts
Develop regular scabies and sores.
Have scabies rates higher than expected.
1. DIAGNOSIS MANAGING CRUSTED SCABIES IN REMOTE ABORIGINAL COMMUNITIES 2014 EDITION 9
2. PATIENT TREATMENT MANAGING CRUSTED SCABIES IN REMOTE ABORIGINAL COMMUNITIES 2014 EDITION 10
Grade Disease Choose best option in each category and add numbers to get score a: distribution and extent of crusting1. Wrists, web spaces, feet only — less than 10% Total Body Surface Area (TBSA)2. As above plus forearms, lower legs, buttocks, trunk OR 10–30% of TBSA 3. As above plus scalp OR more than 30% TBSAb: crusting/Shedding1. Mild crusting (less than 5mm deep), minimal skin shedding2. Moderate (5–10mm deep) crusting, moderate skin shedding3. Severe (more than 10mm deep), profuse skin sheddingc: past episodes1. Never had it before2. 1–3 prior hospitalisations for crusted scabies OR depigmentation of elbows, knees 3. More than 4 prior hospitalisations for crusted scabies OR depigmentation as above PLUS legs/back or residual skin thickening/ scaly skin (ichthyosis) D: skin conditions1. No cracking or pus in skin (pyoderma)2. Multiple pustules and/or weeping sore and/or superficial skin cracking3. Deep skin cracking with bleeding, widespread purulent exudates
(more than 10mm deep),
profuse skin shedding
2. PATIENT TREATMENT MANAGING CRUSTED SCABIES IN REMOTE ABORIGINAL COMMUNITIES
Patients suffer life-long stigmatisation and blame and often avoid health services
1. Identify any fears
Common concerns of crusted scabies patients:
the patient has which
Hospitalisation in an isolation ward.
could be barriers to treatment
Worry about onerous burden involved in whole of household treatment.
Failure of previous treatments reduces motivation to try again and again.
2. Work with patient
Common mistakes in case management of
and family to develop
a treatment plan they
Failing to take time to visit families at home.
are comfortable with
Focusing on clinical protocols before establishing rapport.
Not spending time explaining the disease, its chronicity and the
importance of compliance to break the cycle of recurrences.
Not taking time to win the support of a senior member of the
household to ensure compliance with household treatment.
While it can be frustrating, do not label the patient or family non-
compliant. The family has to be part of the treatment team.
2. PATIENT TREATMENT MANAGING CRUSTED SCABIES IN REMOTE ABORIGINAL COMMUNITIES 2014 EDITION 12
Ideally all patients should be admitted to hospital for treatment (esp. grades 2-3). This is due to risk of sepsis, re-infection from fomites and contacts and infection control. For first diagnosis hospitalisation is especially important as possible underlying immune deficiency needs to be investigated. For community based treatment of crusted scabies at home it is very important that the topical therapy is supervised by the health staff-preferably all doses but especially the first.
Community based treatment: 1. Give ivermectin single dose on days 0, 1, 7. Give with food or milk for better absorption. (N.B. Longer
treatment needed for Grade 2-3. Contact Infectious Disease Team at Royal Darwin Hospital 08 8922 8888 or Alice Springs Hospital 08 8951 7777).
2. Give topical agents (critical part of treatment):
Lactic acid and urea cream (e.g. Calmurid), every second day to soften skin. Don't use on same day as
scabies cream. Applying lactic acid/urea and the next day a warm soaking bath/shower and scrubbing with a sponge is critical for removal of crusts.
Benzyl benzoate 5% with/without tea tree oil OR permethrin every second day for first week.
Dilute benzyl benzoate for children under 12.
THEN twice a week until well. Put on after soaking bath/shower.
3. Patients must be seen daily and linen and clothes must be washed and sunned daily during
2. PATIENT TREATMENT MANAGING CRUSTED SCABIES IN REMOTE ABORIGINAL COMMUNITIES 2014 EDITION 13
Creating a scabies free household
Home visits are critical to gain trust, understanding and
treatment success.
It is important to ensure the household is scabies free to prevent recurrences in the crusted scabies at-
The cycle of transmission can be broken: consistent application of this chronic disease approach improves
quality of life for households and reduces clinical workloads.
2. GRADING AND PATIENT TREATMENT MANAGING CRUSTED SCABIES IN REMOTE ABORIGINAL COMMUNITIES 2014 EDITION 14
Select medications to use
Treat all of the household (scabies cases and contacts) on day 1Repeat for scabies cases only (not contacts) in 1 week.
First line treatments;
Instructions on use of permethrin
Benzyl benzoate has a faster kill time Consider ivermectin in males over
(as per CARPA scabies chapter).
than permethrin and is preferred.
age 5 (NB: STROMECTOL (ivermectin)
is indicated for the treatment of
Do not use in child under 2 months However, it can cause transient burning human sarcoptic scabies when
(use crotamiton e.g. Eurax).
sensation in some patients so give
prior topical treatment has failed or
warning and test on a patch of skin first.
Use in children 2 months and over
is contraindicated.
Instructions on use of benzyl benzoate Treatment is only justified when
25% emulsion (as per CARPA
the diagnosis of scabies has been
Apply thin layer of permethrin 5%
established clinically and/or by
cream on whole body including head
parasitological examination. Without
and face — avoid eyes, mouth.
Apply topically to skin from the neck formal diagnosis, treatment is not
down and leave on overnight.
Requires overnight application.
justified in case of pruritus alone. At all
Do not use in child under 2 years
times follow CARPA Guidelines.
(use permethrin or if under 2 months Comprehensive coverage is critical to
use crotamiton e.g. Eurax cream).
effectiveness of control efforts. Certain
Child 2–12 years and sensitive adults groups in the house may not want to
— dilute with equal parts water (1:1).
use creams, undermining control.
Adults – apply directly.
Consult a medical officer to be part
Benzyl benzoate may occasionally
of the day to consider the use of
ivermectin in men.
cause severe skin irritation, usually Note:
resolves in 15 minutes.
Do not give to women (as ivermectin
Before application, first test on small cannot be used during pregnancy
area of skin.
and pregnancy testing is impractical in community control programs).
Do not give to children under 5.
Dosing of ivermectin :
* Make sure cream covers between fingers and toes, feet including
200mcg/kg rounded up to nearest 3mg.
soles of feet, under nails, buttocks. Leave on overnight and advise
Contact with no clinical scabies-
to reapply after washing hands.
ivermectin Day 1 only
Contact with suspected clinical scabies-
ivermectin on Days 1 and 8.
3. HOUSEHOLD TREATMENT MANAGING CRUSTED SCABIES IN REMOTE ABORIGINAL COMMUNITIES 2014 EDITION 15
Making sure everyone joins in
The application of creams is inconvenient but ensuring all household members use the treatment is critical to the success. Make it a fun occasion and consider the following tips to get everyone involved.
Strategies for success
Take time to get the support and interest of a senior household member. Explain benefits in terms of reduced
sores and improved sleep. It is important to be flexible on the timing.
Select a day and time when most of household will be present (e.g. after school in the afternoon).
Involve senior members of household in helping others apply creams.
Start the application of creams during the home visit. Start by involving mothers to apply creams on children.
Often young children will be frightened. Start with an older person, apply on arms of mothers, staff to get
things started. After initial reluctance a tipping point is reached where everyone joins in. The trick is to stay positive and keep going until you reach this point.
Encourage older teens and adults to help each other with application. Highlight wearing creams as a sign of
their support for household health and wellbeing.
Ensure privacy and appropriate consent before applying creams. Parents should apply creams on children
and be present at all times.
Be discrete. The family may not want the whole community to know they are being treated for scabies.
Screen children and record names of children with scabies. Refer other conditions to health centre
If the family agrees, organise a clean-up for the house. If possible supply cleaning products and equipment.
Encourage household to put bedding, clothes and mattresses in sun.
If it is requested by the family, set insecticide bombs in the house (available over-the-counter in stores).
Ensure families read and understand instructions.
Avoid other health promotion or clinical activities while doing a mini skin day.
3. HOUSEHOLD TREATMENT MANAGING CRUSTED SCABIES IN REMOTE ABORIGINAL COMMUNITIES 2014 EDITION 16
Maintenance plan to prevent recurrences once patient
and family are treated and free of scabies.
4. CHRONIC CARE PLAN MANAGING CRUSTED SCABIES IN REMOTE ABORIGINAL COMMUNITIES 2014 EDITION 17
Ensure a regular supply of creams to patient (e.g. 2 benzyl benzoate, 4 lactic acid/urea (Calmurid) and 4
moisturisers per month) to patient. Breakdown in supply of these creams to patient are a common cause of recurrence.
Only benzyl benzoate should be used for regular preventative treatment (regular use of permethrin or
ivermectin can lead to development of resistance).
Patients should not share a bed and should have a hospital grade mattress which can be easily cleaned
Patients at high risk of re-exposure to scabies are those living in a house with many occupants especially
An intensive phase of clinic involvement is important to show the patient and household the benefit of
adherence to the chronic care plan (e.g sleep).
The patient's seniority in the house is critical. More support is needed for patients without seniority.
* The ultimate goal should be self-care and management with clinics supplying creams
and skin checks.
4. CHRONIC CARE PLAN MANAGING CRUSTED SCABIES IN REMOTE ABORIGINAL COMMUNITIES 2014 EDITION 18
Ongoing management Ongoing management is required after a full treatment of the crusted scabies as per guidelines and where an excellent response has
occured with no evidence of residual active scabies.
Risk of recurrence and
Crusts isolated and
1. Encourage regular
discrete patches — less
use of lactic acid/
than 5% Total Body
including buttocks)
Surface Area (TBSA).
and moisturiser on
Skin: Minimal shedding
areas affected by
Chronicity 0–3 prior hospitalisations for
crusted scabies.
benzoate as needed if exposed to scabies.
Consider supervision of benzyl benzoate.
High infectivity:
1. Encourage regular
Crusts lower legs,
use of lactic acid/
buttocks, trunk OR
including buttocks)
10% or more of TBSA
Skin: Current or past
on areas affected
heavy shedding.
benzoate from neck
More than 3 prior
down fortnightly.
hospitalisations for crusted scabies.
3. As needed apply
And/or depigmentation
of legs/back or residual
skin thickening/ scaly
any areas exposed
to scabies (e.g. hands after visit of affected person).
4. CHRONIC CARE PLAN MANAGING CRUSTED SCABIES IN REMOTE ABORIGINAL COMMUNITIES 2014 EDITION 19
Recurrences are to be expected
Detect, treat early and don't get disillusioned.
Problem-solve with the family as they are part of the treatment team.
Common causes of recurrence include:
- Not treating all contacts.
- Failure to apply creams to hard to reach areas, especially buttocks.
- Running out of supplies of preventative creams.
- Visitors with scabies re-introduce disease to household.
Offer more scabies cream and promote their use with all household contacts.
Consider repeating household treatment and expanding it to include closely related households that could be
source of re-infection.
If scabies persists speak to the One Disease team for program guidance.
At this stage it is more important than ever not to blame the family. In these cases there is normally something else going on and if that can be resolved the scabies will often be fixed by the family themselves. This may just take time and patience.
If many household have scabies consider a Healthy Skin Day. See CDC Healthy Skin Program Guidelines and/or call One Disease for advice.
4. CHRONIC CARE PLAN MANAGING CRUSTED SCABIES IN REMOTE ABORIGINAL COMMUNITIES 2014 EDITION 20
FOR MORE INFORMATION
For clinical advice consult the CARPA standard treatment manual or infectious diseases specialists via the switchboards of Royal Darwin Hospital 08 8922 8888 or Alice Springs Hospital 08 8951 7777.
For information on this document contact One Disease www.1disease.org or [email protected] Scabies ResourcesNT CDC Healthy Skin Program Guidelines (planning a healthy skin day) http://www.health.nt.gov.au/Centre_for_Disease_Control/Publications/CDC_Protocols/index.aspxFlipchart – recognising and treating skin conditions (Menzies) http://www.menzies.edu.au/sites/menzies.edu.au/files/file/research%20pages/Healthy-Skin-Flipchart-Aug09.pdf Developed by program strategy and implementation consultants, EveryVoiceCounts and the One Disease team. Thanks to Prof. Bart Currie for expert advice and pictures used.
Approved by the medical reference group of the East Arnhem Scabies Control Program.
Program design and people empowerment
MORE INFO MANAGING CRUSTED SCABIES IN REMOTE ABORIGINAL COMMUNITIES 2014 EDITION 21
Source: http://www.everyvoicecounts.org/wp-content/uploads/2014/06/Crusted-Scabies-guide-2014.pdf
LA NULIDAD COMO MEDIO DE CONTROL EN LA LEY 1.437 DE 2011 ¿UNA NUEVA INCONSTITUCIONALIDAD? DR. NESTOR RAUL SANCHEZ BAPTISTA Fecha de recepción: 27 de Abril de 2011 – Fecha de aceptación: 1 de junio de 2011 El artículo 137 de la Ley 1.437 de 2011 establece que la nulidad, como medio de control judicial contra los actos administrativos, procede contra los de carácter general y, excepcionalmente, contra ciertos y determinados actos de naturaleza particular y concreta, plasmando así en la ley lo que venía sosteniéndose en la jurisprudencia del Consejo de Estado colombiano, y modificando el postulado general establecido en el artículo 84 del CCA, según el cual la nulidad procede contra todos los actos administrativos definitivos, generales o particulares. Tal concepción jurisprudencial fue considerada contraria a la Constitución Política por la Corte Constitucional con la sentencia C-426 de 2002, en la medida en que era restrictiva del derecho de acceso a la justicia al contener limitaciones no establecidas en la ley. Ahora que fue incorporada a la ley surge el interrogante de si tal inconstitucionalidad fue superada, dado que en los considerandos de aquella se enfatizó en la estrecha relación existente entre la acción de nulidad y el principio de legalidad, para la salvaguarda de la integridad del ordenamiento jurídico sin limitaciones que se consideran constitucionalmente ilegítimas, desproporcionadas e irrazonables. Palabras Claves: Nulidad de actos administrativos, medios de control, guarda de la integridad del ordenamiento, derecho de acceso a la justicia, restricciones legales, inconstitucionalidad. Abstract
Case report of oral melanoma in a king penguin (Aptenodytes patagonicus) found by cooperation between Kosei Inui1, Miyuki Hamaguchi1, Satomi Yonezawa1, Makiko Nishizawa1, Takeshi Wada1, Kazutoshi Takami2 1: Naniwa-Hone-Hone-Dan, Osaka Museum of Natural History 2: Osaka Municipal Tennoji Zoological Gardens AZEC 2013, Fukuoka King penguin (Aptenodytes patagonicus)









