Slide
Program Abstracts
included drowsiness/tiredness (3), increased appetite/weight gain (2),
Background: Recent studies involving Theobroma cacao have shown
mood swings (2) and worsening of headache (2). Flunarizine was
promise in the treatment of a variety of disorders. However, most
discontinued in 17: due to adverse effects in 8 and poor response in 9.
research involving the beneficial effects of cocoa has been limited to
Conclusions: In the cohort studied, Flunarizine appears to be highly
in vitro studies. The balance between inflammatory proteins such as
effective in hemiplegic migraine in comparison to other subgroups.
the MAP kinases (MAPK), and anti-inflammatory proteins such as
In 14% of this group, adverse effects led to discontinuation of Flu-
the MAP kinase phosphatases (MKP) play a critical role maintaining
homeostasis in the trigeminal nociceptive system. It is thought thatan imbalance between MAPK and MKP proteins may play a role inthe pathophysiology of migraine.
Methods: Sprague Dawley rats were fed a control diet or isocaloric
Zonisamide in prophylaxis therapy of the episodic and
diets enriched in cocoa [1% (g/g) or 10% (g/g)] for 14 days prior toan injection of capsaicin or complete Freund's adjuvant (CFA).
chronic cluster headache. An open study
While capsaicin injection mediates an acute inflammatory response,
Pizza V1, Busillo V2 and Agresta A1
CFA was used to cause a chronic inflammatory response. Levels of
1Neuro-Ortho-Traumatology, Neurophysiopathology Unit, Vallo
active ERK, active p38, iNOS, CGRP, MKP-1, MKP-3, and IL-10
della Lucania, Salerno, Italy; 2Interanal Medicine, Neurology
were examined in trigeminal ganglion neurons and glia by immuno-
Unit, Eboli, Salerno, Italy
histochemistry. In addition, total RNA was isolated and then used in
Objectives: To evaluate the efficacy and tolerability of zonisamide in
qPCR to determine the effect of cocoa enriched diets on CGRP
prophylaxis therapy of ECH and CCH.
mRNA levels.
Background: The prophylactic therapy of the episodic (ECH) and
Results: Rats that received injections of capsaicin or CFA were
chronic cluster headache (CCH) is based on verapamil and carboli-
found to have increased levels of staining of the active forms of the
thium. Besides several patients are not responders at this drugs. In
MAPK's ERK and p38 in trigeminal ganglion neurons, while CFA
these cases the use of antiepileptic drug has been proposed. Zonisa-
injections also caused increased expression of the signaling protein
mide, a new antiepileptic drug, has been reported efficacy in the mi-
iNOS, which plays an important role in mediating inflammatory
graineuses patients. The drug has mechanisms of action that suggest
responses. However, the stimulatory effects of capsaicin or CFA on
it may reduce the neuronal hyperexecitability. These mechanisms
these signaling proteins were repressed to basal levels in rats fed
include facilitation of dopaminergic and serotoninergic neurotrans-
cocoa enriched diets. Expression of MKP-1 was increased in both
mission, reduction of glutammate-mediated synaptic excitation and
neurons and glia while MKP-3 and the anti-inflammatory molecule
increased gamma-aminobutyric acid (GABA) release. Zonisamide has
IL-10 were increased only in neurons in rats on a cocoa enriched
a favourable pharmacokinetic profile which includes high oral bio-
diet. Furthermore, rats on cocoa enriched diets exhibited decreased
availability and a long half-life (63 hours), permitting a once or
CGRP mRNA and protein expression in trigeminal ganglion neu-
twice daily dosing regimen. Recent clinical experience indicates a
place for zonisamide in the management of headache disorders.
Conclusions: Cocoa enriched diets are able to repress the stimulated
Methods: 13 patients (pz), (4 F,7 M) mean age 42.8 years (SD 5.8),
expression of proteins associated with the promotion and mainte-
range 36–56 years, suffering from ECH (8pz) and CCH (5 pz)
nance of inflammatory and nociceptive responses. The inhibitory
(ICDH ‘04 criteria) were studied. In all patients with ECH prophy-
effects of cocoa are likely to be mediated via increased basal expres-
laxis therapy with verapamil, carbolithium and valproic acid was
sion of the anti-inflammatory proteins MKP-1, MKP-3, and IL-10.
failed in the past and patients with CCH continued therapy with car-
To our knowledge, this is first evidence for the use of cocoa as a die-
bolithium (2 pz) and verapamil (1 pz). During the three months eval-
tary supplement to cause an upregulation of MKPs and IL-10 as well
uation period zonisamide was administered (starting dose 25 mg/die,
as repress expression of acute and chronic inflammatory responses
target dose 100 mg/die). All patients filled a headache-diary card
within trigeminal ganglia. Importantly, our data also provide evi-
during the evaluation.
dence that cocoa contains biologically active compounds that could
Results: In patients with ECH the basal frequency of attack/days
be beneficial in the treatment of trigeminal-mediated diseases of the
and 1, 2, 3 months respectively was 4.2 (SD 1.9): 2.4 (SD 0.9), 1.6
head and face.
(SD 0.9), 0.8 (SD 1.1) (P < 0.0001). In patients with chronic CH thebasal frequency of attack/days and 1, 3, 6 months respectively was2.8 (SD 1.3): 0.4 (SD 0.3), 0.2 (SD 0.2), 0.1 (SD 0.1) (P < 0.005) (t-
test analysis). In all patients zonisamide was well tolerated (5patients complained somnolence, lack of concentration, vertigo and
Pilot study to assess the efficacy of combining
nausea but not withdrew the study).
valproic acid with a clenching reduction dental splint
Conclusions: These data showed a good efficacy in reduction of fre-
(NTI) as prophylactic treatment for primary headache
quency of attacks. Still, the drug is tolerable, in fact none patients
withdrew the study. Our study suggests that zonisamide could be an
Tarzemany R and Blumenfeld AM
alternative or complementary prophylaxis therapy for ECH andCCH. Controlled studies are warranted to determine the efficacy of
Prosthodontic Department, Azad University, Tehran, Iran
zonisamide in prophylaxis therapy for ECH and CCH.
Objectives: To demonstrate that the combination of medical anddental prophylactic treatments for primary headache disorders willproduce a greater benefit than either treatment alone.
Background: Preventive treatments for migraine and tension type
Repression of acute and chronic inflammatory
headache are often limited by patient compliance and poor tolerabil-
changes in trigeminal ganglion neurons and glia in
ity, as escalating adverse side effects are anticipted as dosages of pre-ventive medications increase. Primary headache disorders have
response to cocoa enriched diets
multiple mechanisms that lead to ongoing headaches and it is likely
Cady RJ and Durham PL
that more than one treatment might be needed in an individual
Center for Biomedical & Life Sciences, Missouri State
patient to control the disorder. To date, there are few studies that
University, Springfield, MO, USA
assess combination treatments in primary headache disorders. In thispilot study we describe a comparative study of the efficacy of noci-
Objectives: To determine the cellular effects of a cocoa-enriched diet
ceptive trigeminal inhibition (NTI) and Valproic acid (VA) in the
on neurons and glia in the trigeminal ganglion under basal condi-
treatment of migraine and tension-type headaches.
tions, and in response to acute or chronic inflammation.
ª 2009 The Authors
Journal compilation ª 2009 Blackwell Publishing Ltd Cephalalgia, 29 (Suppl. 1) (2009) 1–166
Program Abstracts
PO349Sustained efficacy of botulinum toxin type-A (BTXA)on migraine-related disability over 3 treatment cyclesin a community-based settingTurner IM, Harding TM, DeVito DA and Lio RThe Center for Headache Care and Research, IslandNeurological Associates, PC, Plainview, NY, USA
Objectives: To retrospectively assess the effect of botulinum toxintype-A (BTXA) on migraine disability over 3 consecutive treatmentcycles scheduled at 3-month intervals in a community-based head-ache subspecialty practice.
Background: Prior studies using BTXA have shown a decrease inmigraine-related disability, headache days and acute medicationusage. These findings have the potential to result in a substantialreduction in disease burden for patients, employers, insurers andsociety if this is maintained over serial treatment cycles.
Methods: Forty consecutive patients treated for either chronicmigraine (15 or more headache days per month) or high frequencymigraine (8–14 days per month) who underwent 3 consecutive coursesof BTXA treatment at 3-month intervals were retrospectively reviewed.
The primary endpoint was a reduction in Migraine Disability Assess-ment Scores (MIDAS). Secondary endpoints included a decrease inheadache days and as well as a decrease in acute medication use.
Results: Average MIDAS scores decreased from a baseline of 62.8 to29.2 (treatment 1), 31.1 (treatment 2) and 24.8 (treatment 3) over 3consecutive cycles. Headache days decreased from a baseline of aver-age of 20.7 days per month to 11.6 (treatment 1), 9.8 (treatment 2)
and 9.5 (treatment 3) days per month respectively. Monthly acutemedication doses decreased from a baseline average of 51.5 to 27.85(treatment 1), 24.25 (treatment 2) and 21.4 (treatment 3) for the 3cycles of treatment.
Methods: Sixty patients, 18 years of age and older, non-pregnant,
Conclusions: In our retrospective analysis of 40 consecutive patients
who met International Headache Society criteria for migraine and
there was a sustained reduction in migraine-related disability, head-
tension-type headaches were randomly assigned to three treatment
ache days and acute medication use.
groups. 20 patients per treatment arm as follows: Valproic acidalone, NTI splint alone, and combination of NTI and Valproic Acid.
Valproic Acid dose in the treatment arms was 200 mg bid. Clinical
follow-up was performed for 8 weeks at weekly intervals. Thepatients reported headache on a visual analog scale before treatment
Levetiracetam as migraine prophylaxis in topiramate-
and also after every week in their treatment period. Side effects were
reported. Data were collected and compared between the groups
McGreevy K and Gruber A
using the Mann-Whitney and Wilcoxon test.
Headache Clinic, University of California, San Diego,
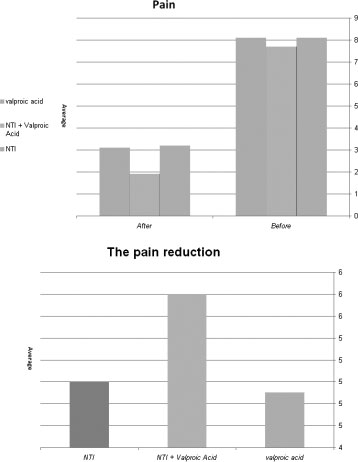
Results: VAS score changes were as follows:
Department of Neurology, San Diego, CA, USA
Valproic acid users showed a 61% reduction in headache. NTI usersshowed a 62% reduction in headache. NTI and Valproic acid users
Objectives: To report a series of topiramate-failures (TFs) who dem-
showed a 76% reduction in headache. The P-value is <0.0001 for
onstrate success with levetiracetam (LVT) for migraine prophylaxis,
the combination treatment compared with either treatment alone.
and to illustrate key characteristics that may be associated with suc-
No side effects reported with the NTI splint. Side effects reported
cess in this subgroup.
for Valproic Acid included: gastro-intestinal upset, alopecia and
Background: Failure
depression. No patients discontinued the study due to adverse
migraine poses an important dilemma for headache specialists. Previ-
ous studies suggest that LVT might be equal to topiramate (TPM)
Conclusions: No statistical difference in treatment efficacy was
but with better tolerability. LVT has a unique mechanism of action.
noted between the Valproic acid and NTI treatment arms. However,
Methods: We present a case series of TFs whose headaches
there was a statically significantly superior improvement for the com-
improved dramatically with LVT. Patients were included with a
bination of Valproic Acid and NTI compared to either of the two
diagnosis of migraine meeting the new IHS classification criteria,
individual treatments. There were no adverse side-effects with the
‡4 days per month of migraine for ‡3 months, and previous treat-
NTI, while side effects were present for patients treated with Valpro-
ment with TPM for ‡3 months. Patients were excluded if they had
ic Acid. Greater therapeutic gain, without an escalation of side
‡20 days per month of migraine for ‡3 months, chronic use of opi-
effects, results from the combination of the two treatments.
ate medication, or an uncontrolled medical condition, including con-current severe depression.
Results: Seven patients with migraine are presented; 2 cases with aura,and 5 without aura. The mean age was 54, with 6 females and 1 male.
The mean number of years with migraine was 20 (range of 5–40). Eachpatient had failed various standard prophylactic treatments includingpropranolol, amitriptyline, verapamil, valproic acid, and in allpatients, TPM, with doses up to 400 mg per day. With respect toTPM, 3 patients discontinued treatment due to intolerable side effectsincluding hair loss, excessive drowsiness, and cognitive slowing, 3 con-tinued treatment and 1 discontinued treatment due to lack of therapeu-
ª 2009 The AuthorsJournal compilation ª 2009 Blackwell Publishing Ltd Cephalalgia, 29 (Suppl. 1) (2009) 1–166
Presented at the 14th International Headache Congress (IHC)
DEPAKOTE with an NTI Clenching Reduction Dental Splint for
Prophylactic Treatment of Primary Headache: A Pilot Study for Efficacy Assessment
Andrew Blumenfeld, MD
Rana Tarzemany, DDS; Morteza Neshandar, DDS;
Nahid Beladimoghaddam, MD
The Headache Center of Southern California,
Ezzatolah Jalalian, DDS
Asst. Professor, Tehran Shahibeheshti Unversity
320 Santa Fe Drive, Encinitas, CA 92024, (760) 631-3000
Dept. of Fixed Prosthodontics, Tehran Azad University
Emam Hosein Hospital, Neurology Ward
Background – The NTI (Nociceptive Trigeminal Inhibition) intraoral device reduces maximum nocturnal trigeminal motor
hyperactivity (jaw clenching), and is hypothesized to therefore reduce resultant noxious afferent activity. The NTI has been FDA
approved for the prophylactic treatment of medically diagnosed migraine pain.
Nocturnal Motor Hyperactivity (Clenching)
Normal Nocturnal Motor Activity (with
1. Hyperactive temporalis
2. Hyperactive lateral pterygoid
1. Minimal y intense temporalis activity
Resultant Sensory Nociception
A) Muscle strain and
Resultant Sensory Nociception
B) Joint strain and load
C) Facial / sinus tension
A) Minimal noxious input
D) Periodontal ligament compaction
An NTI device is custom made by a
dental professional, providing only for
incisor-edge contact with minimal
jaw-opening (to minimize TMJ strain)
Molar and canine tooth contact allows for pathologic intensity of
Providing for only incisor-edge contact with an NTI device
trigeminal motor hyperactivity (nocturnal jaw clenching)
minimizes trigeminal nociception.
In a previous study (presented at the Headache and Migraine Trust International Congress 2008), 20 consecutive refractory CDH patients
treated in a headache center, all scoring "severe and disabling" on their HIT-6 questionnaire despite maximal oral prophylactic medication,
were properly fitted with an NTI device and wore nightly for 9 months.
Within two months of nightly NTI use, and then persisting for the nine months of observation, half of the subjects had a significant
improvement, while 25% reported that chronic headache no longer had any impact on their lives.
DEPAKOTE (valproic acid) is FDA approved for prophylactic treatment of migraine.
The adverse events with Valproic acid treatment include: weight gain, fatigue, alopecia, hirsutism, tremor, and liver function
abnormalities. Most of the side effects are dose related and worsen with higher doses.
Methods: 60 patients, 18 years of age and older, non-pregnant, met IHS criteria for migraine and tension-type headaches;
randomly assigned to three treatment groups, 20 pts per arm: Valproic acid alone, NTI splint alone, and combination of NTI and
Valproic Acid. Valproic Acid dosage in the treatment arms was 200 mg bid. Clinical follow-up was performed for 8 weeks at
weekly intervals. The patients reported headache on a visual analog scale before treatment and also after every week in their
treatment period. Side effects were reported. Data collected and compared between the groups using the Mann-Whitney and
Wilcoxon test.
Results: There was a statically
significantly superior improvement for the
combination of Valproic Acid and NTI
compared to either of the two individual
treatments, with no statistical difference in
treatment efficacy between the Valproic
Depakote + NTI
acid and NTI treatment arms. There
were no systemic adverse side-effects
with the NTI, while side effects were
present for patients treated with Valproic
Acid but did not worsen when combined
with the NTI.
Conclusion: The known therapeutic
gain of Valproic Acid can be increased
without risking the escalation of the known
side effects of increasing dosage, by
combining Valproic Acid with the proper
use of an NTI device.
Source: http://www.kellerlab.com/wp-content/uploads/2015/11/Blumenfeld-09.2009.pdf
Revista de laAsociación Madrileña de Veterinarios de AMVAC Animales de Nº 5 - Septiembre - Octubre 2004 dermatosis faciales caninasUn enfoque práctico y sistemático de estos problemas Aproximación a laEhrlichiosis caninaUna revisión completa y actual desde su etiología hasta su tratamientoVetMADRID 2005"Medicina y Cirugía del Aparato Locomotor" distintas fÓrmulas jurídicas paracrear una empresa¿Cuál es la forma jurídica más apropiada para crear una empresa?Honorarios Mínimos OrientativosComparativa entre los distintos Colegios Provinciales que los publican
Psychiatric Medications and School Shooters Peter Langman, Ph.D. There is a widespread belief that an "epidemic" of psychiatric effects. Medications can also have withdrawal effects, meaning medications is causing an "epidemic" of violence, particu- that people have adverse reactions when they stop taking the larly in students. Some who hold this belief also believe that


