Slide

Understanding Diabetes
And Your Risk
Presented by:
Sheryl Bartholow, FNP-BC
Family Medicine
10/13/2014

Important Notice
The information contained in this document is for informational purposes only. It is not intended to diagnose or treat specific patients and should not be used as a substitute for the medical care and advice of your health care provider. In addition, this document may contain references to specific products and/or medications. Such references, whether by brand name or generically, are provided for informational purposes only and do constitute endorsement, recommendation, or approval by GRHS or its medical providers. Always consult a medical professional if you have concerns regarding your health. If you are experiencing a medical emergency, dial 911.
Some images have been removed from the original presentation due to copyright or other considerations.

3 Main Points
How can you decrease your risk of
What is the difference between
diabetes and pre-diabetes?
What can you expect if you develop
either condition?


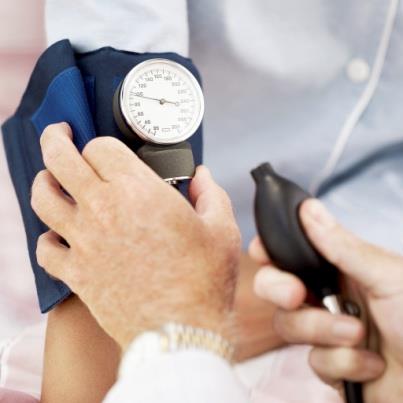
Risk factors for diabetes
Over 40 years old Overweight Family history Diabetes during pregnancy Baby over 9 lbs. Stress of illness or injury Elevated blood pressure Sedentary Lifestyle Some minorities

How to decrease risk of Diabetes
Stay at a healthy weight -BMI 19-25 Eat well: healthy fats, lean proteins, lots of
fruits and vegetables, low-fat dairy
Be active: preferably 30 minutes at least 3
With these steps, you can stay healthier
longer and lower your risk of diabetes.
From the ADA web page,
www.diabetes.org

When fasting blood sugar is between 100-
When HgbA1c is between 5.7-6.4 When oral glucose tolerance test shows
blood sugar between 140-199
Pre-diabetes cont.
Sometimes occurs with symptoms of
Many times it has no symptoms Always occurs before type II diabetes, but
diabetes doesn't always have to follow it
Pre-diabetes cont.
Losing 7% of body weight (15# for
someone who's 200#) can lower risk of Type II diabetes being diagnosed
Exercising 30 minutes 5 times weekly can
decrease risk of diabetes diagnosis
With pre-diabetes it is important to be
checked for Type II diabetes every 1-2 years
Signs and Symptoms of Diabetes
Tired Dry itchy skin Numbness or tingling in hands or feet Increased urination Problems with sexual function Slow healing Increased thirst Unexplained weight loss
What can you expect if you develop
diabetes?
5 main points for Controlling
Type II Diabetes
Blood Glucose testing
Diet
Exercise
Medications
Visits with Health Care providers
Overview of Diabetes
24 Million people with diabetes in USA 3 types of diabetes
Type 1 (auto-immune, NO insulin) Type 2 (insulin resistance & insulin deficiency) Gestational (pregnancy hormones= I.R.)
"Pre-diabetes" (also has risk factors)
Target Glucoses for Diabetics
70-120 mg/dL premeal Less than 160 mg/dL
(2 hours post prandial)
A rise of less than 40
(2 hours post prandial) if on Rapid acting insulin (Humalog, Novolog, or Aspart)
Blood Glucose Testing
ALL people with diabetes should test
If no meds or pills
test BG 3 x/day (minimum 2-3 days per week)
If on insulin
prefer 4 x/day test as often as Health Care Provider or
educator asks you to
The Natural History of Type 2 Diabetes
Post Meal Glucose
Fasting Glucose
Insulin Resistance
Functi 100
Insulin Level
At risk for Diabetes
Beta cell failure
Years of Diabetes
Abnormal Glucose Metabolism
Glucose Metabolism
Peripheral tissues
(Muscle and Fat)
Improper regulation of
(Type 1 and Type 2)
Relative Insulin deficiency
(Type 2) or no insulin (Type 1)
What is Type II?
Beta cells struggling
to produce enough insulin to overcome insulin resistance.
Complications from high blood glucose
Retinopathy-diabetes affects eyes Neuropathy- nerve cells swell and scar Nephropathy-diabetes affects kidneys Cardiovascular- higher risk of heart
disease, especially with abnormal cholesterol, high blood pressure, smoking
Carbohydrate Counting
What is a carbohydrate? Carbohydrate raises blood sugar Examples of carbohydrates (CHO)
Bread, starch, milk, fruit, sweets
15 Gms of CHO = 1 choice Recommend from 3(-5) choices per meal
What is a Carbohydrate?
Any food that turns to sugar after it is
eaten is considered a carbohydrate
Starches and grains - Bread, potatoes, pasta,
Fruits and fruit juices Milk and yogurt Sweets
What foods are not considered
carbohydrates?
Most vegetables Meats and meat substitutes Fats
Exercise and Diabetes
Primarily applies to Type II In Type I, an individualized approach with
health care provider/educator is usually needed
Important to start moving more -stairs,
parking further away from destination, going for a walk
Start slow or increase current exercise
Exercise cont.
Find times that work into your schedule so
you can be consistent
Check blood sugar before and after
vigorous exercise, especially when beginning program
Carry fast acting carbohydrate (juice,
glucose tabs) with you during vigorous exercise
Medications
Discuss medication options with Health
Insulin –always in Type I, sometimes in
Type II, esp. when disease present longer
Sulfonylureas –glipizide (Glucotrol),
glimepiride (Amaryl), glyburide-stimulate pancreas to release more insulin
Biguanides –metformin (Glucophage)-
decreases amount of glucose made by liver
Medications cont.
Meglitinides –repaglinide (Prandin),
nateglinide (Starlix)-stimulate pancrease to secrete more insulin
Thiazolidinediones –rosiglitazone (Avandia),
pioglitazone (Actos)-help insulin work better in muscle and fat and decrease glucose from liver
DPP-4 inhibitors -the "gliptins" like Januvia
and Onglyza-prevents breakdown of GLP-1 in body, which regulates blood glucose
Medications cont.
SGLT2 inhibitors- Invokana and Farxiga-let
excess glucose pass out of body into urine
Alpha-glucosidase inhibitors –acarbose
(Precose), meglitol (Glyset)-blocks the breakdown of starches and slows breakdown of sugars
Bile acid sequestrants -
colesevelam(Welchol)-binds with bile acids in digestive system, lowers cholesterol and blood glucose
Medications cont.
GLP-1 Receptor Agonists - exenatide
(Byetta), liraglutide (Victoza), pramlintide (Symlin) –normalize blood glucose, makes you feel full longer and helps insulin in your body work better. Many lose weight. It is injectable.
New once weekly versions- dulaglutide
(Trulicity), albiglutide (Tanzeum), exenatide (Bydureon)
How often do I need to see my
health care provider?
EVERY 3 MONTHS!! Visit to include:
HgbA1c Foot check
Annual visit to include:
Comprehensive foot exam Lipid profile Urine screening for protein Stress test (every 5 years)
What should I bring?
LOG BOOK!! Log book should include:
Blood sugars with dates & relationship to
Exercise Medications (esp. if on insulin) Results of previous test results (ie. HgbA1c,
lipids, urine screening for protein, etc.)
Any questions for provider written down
ABC's of Self-Management
(Hemoglobin) A1c <7% (as close to 6% as can get)
Blood Pressure < 130/80
Cholesterol (LDL<100)
Blood glucose (BG) control is
BG testing improves BG
See your physician every 3
Bring your LOG BOOK!! Remember your A, B, C's!
Questions?
Source: http://grhsonline.org/wp-content/uploads/2010/03/Understanding-Diabetes-Risk-Web.pdf
ECUADOR DATASHEET LAST MODIFIED 22.05.2008 1. PRESHIPMENT INSPECTION (PSI) MANDATE: Corporación Aduanera Ecuatoriana (CAE) All goods shipped until and including February 29, 2008 shall be subject to PSI. NNRFs (Avisos de No Conformidad) shall be issued in case final documents are not received within 15 working days from the
Movimientos anormales Pilar Guerrero, MD Neuróloga infantil Hospital Militar Nueva Granada Universidad Militar Nueva Granada Los desórdenes del movimiento son la mani- vía piramidal, por consiguiente, no se deben festación clínica de síndromes que involucran a una enfermedad cerebrovascular, ni a una no solo movimientos involuntarios anormales enfermedad por sí misma del cordón espinal, en sí, sino compromiso en la realización de un









